- Upper abdominal pain shows up in the area between your ribcage and belly button.
- This region houses your stomach, liver, gallbladder, pancreas, and parts of your intestines.
- The pain can feel sharp, dull, burning, or cramping.
- It might last minutes or stick around for days.
- The location tells you which organ might be struggling.
What Is Upper Abdominal Pain?
Upper abdominal pain means any discomfort you feel in the top section of your belly. Everything above your belly button, stretching up to where your ribs meet, counts as your upper abdomen. This includes the space right beneath your breastbone and spreads out to both sides under your lower ribs.
Your upper abdomen packs in several vital organs, such as the stomach, liver, gallbladder, and duodenum (the first part of your small intestine). When any of these organs run into trouble, you feel upper abdominal pain in specific patterns.
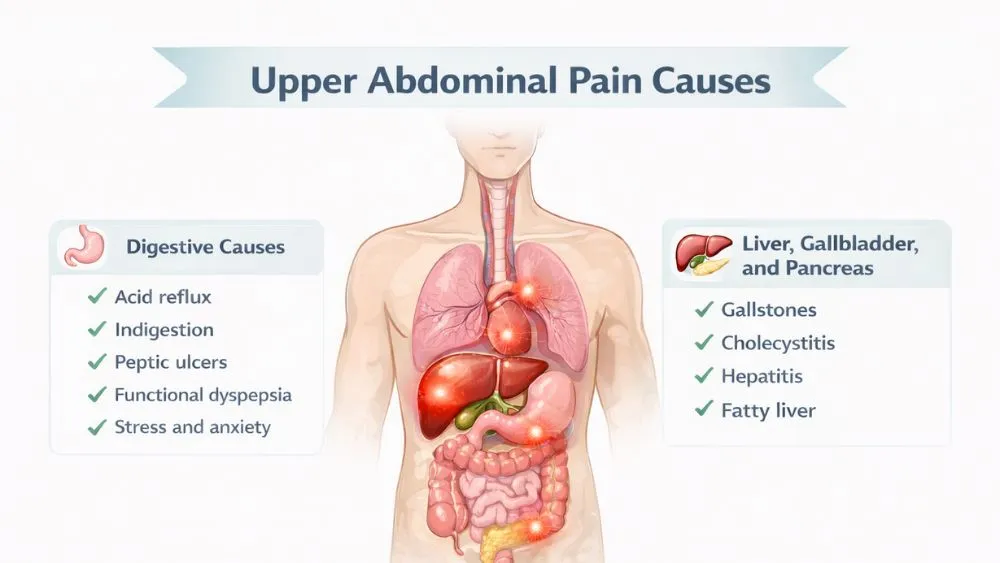
Upper Abdominal Pain Causes

Your digestive system is a major cause of upper abdominal pain. Your gallbladder and liver rank second for causing trouble. Problems with your pancreas come third but tend to be more serious. Occasionally, issues outside your digestive system create belly pain too.
Digestive Causes
Acid reflux happens when stomach acid flows backward into your esophagus (the tube connecting your mouth to your stomach). This creates burning upper abdominal pain right under your breastbone. You may taste sour liquid in your mouth or feel like food is coming back up.
Gastritis means the protective lining inside your stomach gets inflamed or damaged. When that layer breaks down, acid irritates the stomach tissue underneath. The resulting upper abdominal pain feels like gnawing or burning in your upper belly center.
Indigestion (dyspepsia) creates uncomfortable fullness and upper abdominal pain without any visible damage to your organs. You feel bloated, need to burp constantly, and sometimes get nauseated. Eating too much, eating too fast, or eating while stressed commonly triggers this.
Peptic ulcers are sores that form in your stomach lining or the beginning of your small intestine. Ulcer pain typically strikes when your stomach is empty because there’s no food to buffer the acid. You may wake up between midnight and 3 AM with pain. Eating temporarily helps, but the pain returns a few hours later.
Functional dyspepsia affects people whose digestive system looks completely normal on tests but still causes upper abdominal pain. Your gut nerves overreact to normal amounts of acid or stretching. Your brain receives exaggerated pain signals from normal digestive processes. Stress and anxiety make this hypersensitivity worse.
Liver, Gallbladder, and Pancreas Causes
Gallstones form when substances in bile (a digestive fluid made by your liver) harden into pebble-like pieces. This creates sudden, intense upper abdominal pain on your right side. Attacks typically start 30 minutes to two hours after eating greasy meals. The pain can last 15 minutes or continue for several hours.
Cholecystitis means your gallbladder gets inflamed, usually because a gallstone gets stuck. Your gallbladder swells and might even get infected. Fever often develops. The pain stays severe and pressing on your right upper belly really hurts.
Hepatitis refers to liver inflammation. Viruses cause most cases (hepatitis A, B, or C), but alcohol abuse, medications, or autoimmune conditions also trigger it. Hepatitis causes persistent, achy discomfort. Your skin and eyes might turn yellow (called jaundice). Your urine turns dark brown.
Fatty liver disease happens when fat builds up inside liver cells. As the condition advances, you might notice discomfort or fullness in your upper right abdomen. Obesity, diabetes, and heavy alcohol use cause this condition.
Pancreatitis means your pancreas gets inflamed. This creates severe upper abdominal pain in your center that often radiates straight through to your back. The pain gets worse after eating and when lying flat. Sitting up and leaning forward sometimes helps. Gallstones and heavy alcohol use cause most cases.
Pancreatic insufficiency happens when your pancreas doesn’t make enough digestive enzymes. You get upper abdominal pain, bloating, and oily stools that float.
Serious Causes That Need Urgent Care
Perforated ulcers occur when a stomach ulcer burns completely through the stomach wall. This creates sudden, extreme upper abdominal pain that spreads across your whole belly. Even gentle touching causes severe pain. This medical emergency needs surgery.
Gastric outlet obstruction happens when something blocks the exit from your stomach. You vomit undigested food from meals you ate hours earlier.
Abdominal aortic aneurysm is a weak, bulging spot in your main artery. If it tears or ruptures, you get catastrophic upper abdominal pain with severe back pain. This kills quickly without emergency surgery.
Stomach cancer grows slowly and often causes no symptoms early on. As it advances, you get persistent upper abdominal pain, feel full after tiny amounts of food, and lose weight without trying. Blood might appear in your stool, turning it black and tarry.
Heart attacks sometimes create upper abdominal pain instead of chest pain, especially in women. If your belly pain comes with sweating, shortness of breath, nausea, or pain spreading to your jaw or arm, call emergency services immediately.
Upper Abdominal Pain Symptoms
Upper abdominal pain symptoms rarely show up alone. Your body sends multiple signals at once because different systems connect and influence each other.
Mild and Common Symptoms
Bloating makes your belly swell up and feel tight like an overfilled balloon. Sometimes your belly makes gurgling or rumbling sounds as gas tries to move through.
Burning sensations start deep in your upper belly and sometimes travel upward toward your throat. The burn feels similar to swallowing something hot. Acid reflux causes most burning upper abdominal pain.
Fullness after eating just a few bites happens when your stomach can’t empty properly. Sometimes inflammation makes your stomach extra sensitive to stretching.
Belching releases swallowed air from your stomach. Everyone burps occasionally, but excessive belching points to digestive trouble. You might be swallowing air while eating too fast, drinking carbonated beverages, or feeling anxious.
Severe Symptoms You Should Not Ignore
Persistent pain lasting beyond three days without improvement needs evaluation.
High fever combined with belly pain means infection somewhere. Your temperature climbs above 100.4°F.
Vomiting that won’t stop for more than 12 hours leads to dehydration fast. You can’t keep down water, food, or medications. Your mouth gets dry and sticky. You pee less frequently and your urine turns dark yellow. Blood in vomit looks either bright red or like coffee grounds (partially digested blood).
Unexplained weight loss means dropping pounds without changing your diet or exercise habits.
Upper Abdominal Pain After Eating
Upper abdominal pain after eating affects millions of people daily. Any hiccup in your digestion triggers pain. The timing between eating and pain onset tells you a lot about where the problem sits.
Why Pain Starts After Meals
Your stomach releases hydrochloric acid within minutes of food arriving. This acid is strong enough to dissolve metal, but your stomach lining normally handles it fine.
- If you have gastritis, ulcers, or a damaged stomach lining, this acid surge burns exposed tissue. Pain typically begins 15 to 60 minutes after eating.
- If gallstones partially block the duct, this creates sudden, intense upper abdominal pain after eating on your right side. The pain peaks quickly, often within 30 minutes of finishing a fatty meal.
- Gas production increases after eating certain foods. When gas gets trapped, pressure builds and causes cramping upper abdominal pain. The pain moves around as gas travels through your intestines.
Your stomach stretches as it fills with food and liquid. Normally, this stretching feels comfortable. But if you eat too fast, your stomach doesn’t have time to signal your brain that you’re full. The excessive stretching creates uncomfortable pressure and pain. If you eat while distracted (watching TV, working), you eat too much before your body can warn you.
Foods That Commonly Trigger Pain
Fatty foods require the most digestive effort. Fried chicken, french fries, creamy pasta dishes, cheese-heavy meals, and fatty cuts of meat.
Spicy foods contain compounds like capsaicin that directly irritate your stomach lining. Hot peppers, curry dishes, hot sauce, and heavily seasoned foods trigger burning pain.
Alcohol damages your stomach lining in multiple ways. Hard liquor hits hardest, but wine and beer cause problems too. Drinking on an empty stomach magnifies the damage.
Oranges, grapefruits, lemons, tomato sauce, and salsa all have pH levels similar to stomach acid. If you already have reflux or gastritis, these foods pour more acid on irritated tissue.
Caffeine stimulates your stomach to produce extra acid. Coffee is the biggest offender, but tea, energy drinks, and some sodas contain significant caffeine too.
Upper Abdominal Pain and Nausea
Nausea is that queasy, unsettled feeling in your stomach that makes you not want to eat. It often comes right before vomiting but can linger for hours without leading to actual vomiting. When pain and nausea hit together, your digestive system is usually struggling with inflammation, infection, or blockage.
What Pain With Nausea Usually Indicates
Stomach irritation from viral infections creates both symptoms simultaneously. You get cramping upper abdominal pain and nausea along with diarrhea.
Gallbladder problems frequently combine pain with waves of nausea. You might vomit bile (a yellow-green bitter fluid). Unlike stomach contents, bile comes from your liver and tastes extremely bitter.
Food poisoning happens when you eat something contaminated with bacteria or toxins. You get severe cramping, upper abdominal pain and nausea, followed by vomiting and diarrhea.
Medication side effects upset your stomach chemistry. Antibiotics kill beneficial gut bacteria along with harmful ones, disrupting digestion. Iron supplements irritate your stomach lining. Pain medications called NSAIDs (like ibuprofen) damage your stomach’s protective layer.
When Nausea Makes Pain More Concerning
Dehydration happens fast when you can’t keep fluids down. Within hours, you get dizzy when standing up. You pee infrequently and what comes out is dark yellow or amber colored.
Persistent vomiting beyond 24 hours strips your body of important electrolytes like potassium, sodium, and chloride. This becomes especially dangerous for people taking critical medications for conditions like diabetes or heart disease.
Blood in vomit means you’re bleeding somewhere between your mouth and upper intestine. Any blood in vomit needs immediate medical evaluation.
Upper Abdominal Pain Gas
Upper abdominal pain gas creates sharp, cramping discomfort that comes and goes in waves. Gas is normal, everyone produces it. Adults produce one to four pints of gas daily and pass gas 14 to 23 times per day on average. Problems start when gas gets trapped or when you produce excessive amounts.
How Gas Causes Upper Abdominal Pain
Trapped air in your stomach creates pressure against your stomach walls and diaphragm (the muscle separating your chest from your abdomen). This pressure triggers pain receptors. The pain feels sharp and cramping. It might make breathing feel uncomfortable. Burping releases this trapped air and provides instant relief.
Slow digestion gives bacteria more time to ferment food in your intestines. The longer food sits in your intestines, the more gas bacteria produce. This creates bloating and cramping upper abdominal pain gas that builds throughout the day.
Swallowing air happens more than you realize. You gulp air when eating too quickly, drinking through straws, chewing gum, sucking on hard candy, or drinking carbonated beverages. This air needs to exit somehow, either through burping or traveling through your entire digestive tract to exit as flatulence.
How to Differentiate Gas From Serious Pain
Gas pain moves around your abdomen instead of staying fixed in one spot. You might feel it on your left side, then five minutes later it shifts to your right side or center. This migration happens as gas bubbles travel through your intestines. Serious conditions like appendicitis or gallstones create pain that stays in the same location.
When you release trapped air by burping, the pressure disappears and pain vanishes immediately. If pain persists unchanged after passing gas, something else is causing it.
Gas pain rarely comes with fever, bloody stools, severe weight loss, or persistent vomiting. These red-flag symptoms indicate problems beyond simple gas.
How Upper Abdominal Pain Is Diagnosed
Doctors follow a systematic approach to figure out what’s causing your upper abdominal pain. The process starts with questions and a physical exam, then progresses to tests only if needed.
Your doctor asks detailed questions about your pain.
- When did it start? Where exactly do you feel it?
- Does it stay in one spot or move around?
- What does it feel like (sharp, dull, burning, cramping)?
- What makes it better or worse? Does eating affect it?
- Any other symptoms like fever, vomiting, or weight changes?
Your answers create a pattern that points toward specific organs or conditions.
Your doctor looks at your skin and eyes for yellowing. They press on different areas of your abdomen checking for tenderness, swelling, or masses. Pressing then quickly releasing (rebound tenderness) tests for inflammation.
- Blood tests reveal inflammation, infection, and organ function.
- Ultrasounds work great for viewing gallstones, liver problems, and pancreas inflammation.
- CT scans are best for detecting infections, tumors, and complications.
- X-rays show less detail but can reveal blockages or perforations.
- Endoscopy reveals ulcers, inflammation, bleeding, or tumors.
Treatment Options for Upper Abdominal Pain
Treatment for upper abdominal pain targets the underlying cause, not just the symptom. Your doctor matches treatment to your specific diagnosis.
Home and Lifestyle Measures
Diet modifications prevent many types of upper abdominal pain. Identifying and avoiding trigger foods stops symptoms before they start. Keep a food diary tracking what you eat and when pain occurs.
Eating smaller, more frequent meals reduces stomach workload. Eating five or six small meals spreads digestive work throughout the day. Stop eating at least two to three hours before lying down so gravity helps keep stomach contents down.
Staying upright after meals prevents acid reflux. Don’t lie down, bend over repeatedly, or exercise vigorously right after eating.
Hydration supports every aspect of digestion. Aim for clear or pale yellow urine as a sign of good hydration.
Stress management directly impacts digestive function. Deep breathing exercises, meditation, gentle yoga, or regular walks calm your nervous system and reduce upper abdominal pain triggered by stress.
Medical Treatment
Antacids neutralize existing stomach acid for quick symptom relief. Brands like Tums, Rolaids, or Maalox help occasional heartburn or indigestion.
H2 receptor blockers reduce how much acid your stomach produces. Famotidine and ranitidine cut acid production by about 70% and work for 12 hours. They take 30 to 90 minutes to start working but provide longer relief than antacids.
Proton pump inhibitors provide the strongest acid suppression. Omeprazole, lansoprazole, and esomeprazole reduce acid production by 90% or more. They take one to four days to reach full effectiveness but work for 24 hours per dose. Doctors prescribe these for severe reflux, ulcers, or gastritis.
Enzyme supplements help when your pancreas doesn’t make enough digestive enzymes. Pancrelipase helps if you have chronic pancreatitis or pancreatic insufficiency.
When to See a Doctor for Upper Abdominal Pain
Most belly pain resolves on its own within hours. Simple gas, minor indigestion, or eating too much rarely need medical attention.
- Pain persisting beyond 24 hours without improvement deserves evaluation.
- Pain so severe you can’t stand upright or find any comfortable position requires emergency care.
- Fever above 101°F with upper abdominal pain suggests infection.
- Vomiting blood (bright red or coffee-ground appearance) indicates bleeding.
- Chest pain, difficulty breathing, or pain radiating to your shoulder or jaw.
- Yellowing skin or eyes.
- Severe tenderness when touching your abdomen, especially with a rigid, board-like belly.
- Pregnancy with abdominal pain always needs evaluation to rule out ectopic pregnancy or other complications.
- Abdominal pain after an injury might indicate internal bleeding or organ damage.
FAQs About Upper Abdominal Pain
Is upper abdominal pain serious?
Not usually, but it can be. Most upper abdominal pain comes from gas, indigestion, or minor stomach irritation that resolves quickly. However, persistent pain lasting days, severe pain preventing normal activities, or pain with fever, vomiting blood, or jaundice requires immediate medical evaluation.
Can upper abdominal pain be caused by gas only?
Yes, gas alone frequently causes upper abdominal pain. The key difference is gas pain moves around, improves after burping or passing gas, and responds to walking. Pain from serious conditions stays fixed in one location and persists despite releasing gas.
Does upper abdominal pain always mean a stomach problem?
No. While stomach issues cause most cases, upper abdominal pain can originate from your liver, gallbladder, pancreas, or even heart. Right-sided pain often indicates gallbladder or liver problems. Central pain frequently involves stomach or pancreas. Left-sided pain might come from stomach or spleen.
Is upper abdominal pain after eating normal?
Mild fullness is normal, but significant upper abdominal pain after eating is not. Sharp pain, burning, or nausea after regular meals indicates problems like gallstones, gastritis, ulcers, or reflux. Pain starting 30-120 minutes after fatty foods strongly suggests gallbladder disease. Burning within an hour points to acid problems.
Can stress cause upper abdominal pain?
Absolutely. Stress directly affects your gut through the brain-gut connection. Anxiety increases stomach acid production, slows digestion, and makes pain nerves hypersensitive. However, don’t assume all pain is stress-related without ruling out physical causes through proper medical evaluation.
Is upper abdominal pain related to liver disease?
Sometimes. Your liver is in your right upper abdomen, so liver inflammation from hepatitis or fatty liver disease causes pain there. However, early liver disease often produces no pain. Upper abdominal pain with yellowing skin, dark urine, pale stools, or extreme fatigue strongly suggests liver involvement requiring immediate medical attention.
Can upper abdominal pain go away on its own?
Often yes. Upper abdominal pain from gas, overeating, or mild indigestion typically resolves within hours as your body processes food and releases trapped air. However, pain lasting more than 24 hours or recurring frequently needs medical evaluation.
Is upper abdominal pain different from lower abdominal pain?
Yes, because upper abdominal pain typically involves stomach, liver, gallbladder, or pancreas problems. Lower abdominal pain more commonly relates to intestines, appendix, bladder, or reproductive organs.
Can upper abdominal pain be a sign of cancer?
Rarely, but yes. Cancer pain typically starts mild and gradually worsens over weeks or months. It comes with unexplained weight loss (10+ pounds without trying), loss of appetite, extreme fatigue, or feeling full after tiny meals.
When should upper abdominal pain not be ignored?
Never ignore upper abdominal pain with warning signs, including severe intensity preventing normal activities, duration exceeding three days, fever above 101°F, vomiting blood, black tarry stools, chest pain or breathing difficulty, yellowing skin or eyes, rigid board-like abdomen, or pain after injury.












Leave a Comment