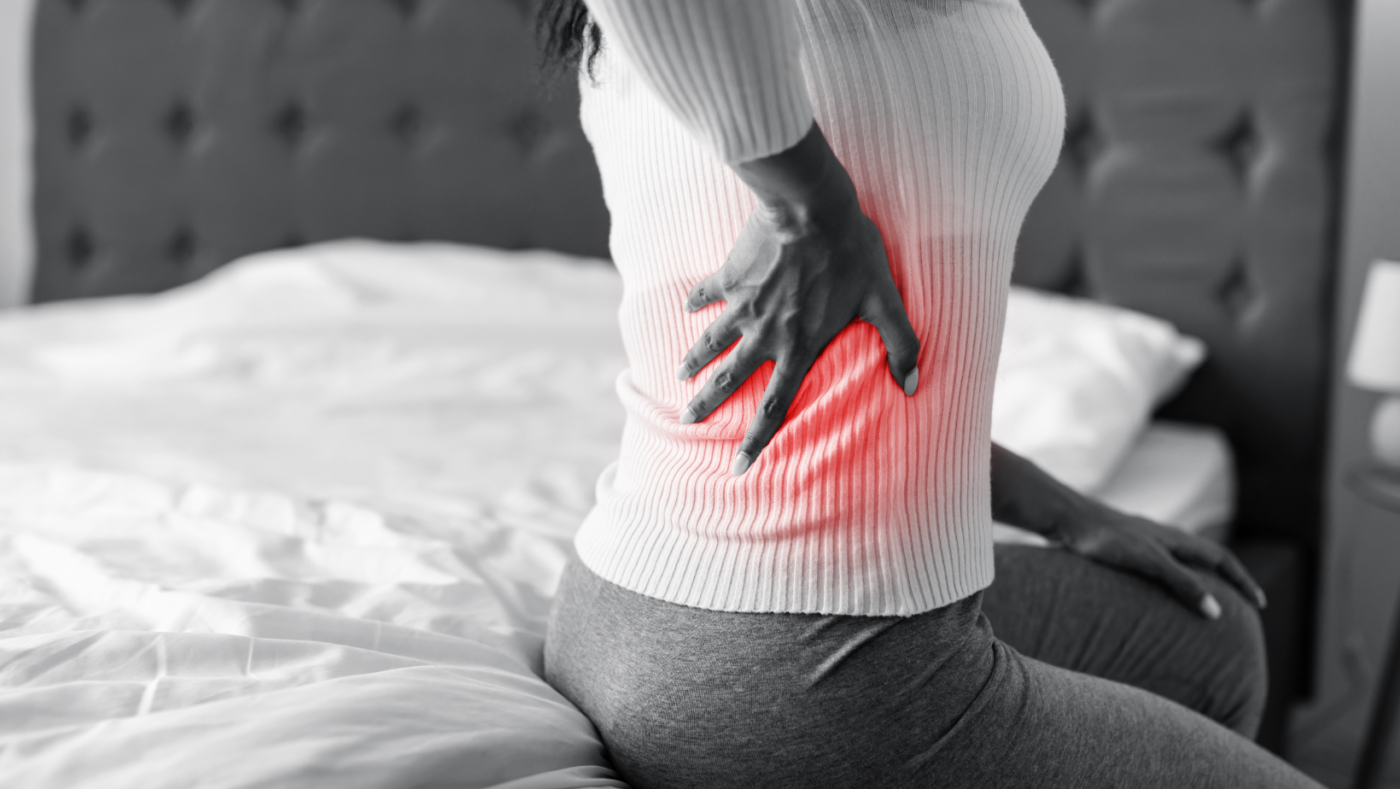
Back pain is the leading cause of disability worldwide. The Global Burden of Disease study ranks it as the single biggest contributor to years lived with disability across 195 countries. Nearly 80% of adults experience it at some point in their lives.
What Is Back Pain?
Back pain is discomfort anywhere along the spine, from the neck down to the tailbone. It ranges from a dull ache to sharp, stabbing pain. The spine is made up of vertebrae, discs, muscles, ligaments, and nerves. When any of these get damaged, irritated, or compressed, pain follows.
Most back pain (about 85% of cases) has no specific structural cause. Doctors call this “non-specific back pain.” It’s real, it hurts, and it responds well to movement and basic treatment.
How to Tell if Back Pain Is Muscle or Organ?
This distinction matters, and most people get it wrong.
Muscle back pain:
- Gets worse with movement, bending, or twisting
- Feels better with rest or heat
- Often follows physical activity or a sudden awkward movement
- Tender to the touch on the back surface
- Usually dull or achy
Organ-related back pain:
- Doesn’t change with movement or rest (it hurts regardless of position)
- Comes with other symptoms like fever, nausea, painful urination, or bloating
- Often feels deeper, inside the body rather than on the surface
- Doesn’t improve with pain relievers like ibuprofen
Kidney pain is just below the rib cage on one side. Muscle pain sits more centrally or spreads across the lower back. If the pain doesn’t follow activity and comes with any systemic symptoms, get it evaluated.
What Is the Cause of Lower Back Pain?
Lower back pain has six common causes:
- Muscle or ligament strain: The most frequent cause. Lifting incorrectly, sudden movements, or long periods of poor posture strain the soft tissues around the lumbar spine.
- Herniated disc: The gel-like cushion between vertebrae pushes outward and presses on nearby nerves. This causes sharp, shooting pain that often travels down one leg (called sciatica).
- Degenerative disc disease: Discs shrink with age, reducing cushioning. Common after 40.
- Spinal stenosis: The spinal canal narrows and compresses nerves. Causes pain, numbness, or weakness in the legs during walking.
- Facet joint problems: Small joints in the spine that stabilize movement become inflamed or arthritic.
- Sacroiliac joint dysfunction: The joint connecting the spine to the pelvis gets inflamed, causing deep lower back or buttock pain.
What Are the Risk Factors for Back Pain?
The factors that raise back pain risk the most are:
- Sedentary lifestyle: Sitting for long hours weakens core muscles that support the spine
- Age: Disc degeneration starts in the 30s and accelerates after 50
- Excess body weight: Every extra pound adds pressure to lumbar discs and joints
- Smoking: Reduces blood flow to spinal discs, speeding up degeneration
- Physically demanding jobs: Repeated heavy lifting, bending, or whole-body vibration (truck drivers, construction workers)
- Psychological stress: Chronic stress increases muscle tension in the back and raises pain sensitivity
- Prior back injury: The single strongest predictor of future back pain
What Causes Sudden Pain in the Lower Back?
Sudden lower back pain that hits without warning usually has one of three causes.
The first is a muscle spasm. The back muscle contracts suddenly and won’t release. This happens during lifting, twisting, or even sneezing. It feels like a sharp lock in the back.
The second is a disc herniation. A disc can rupture during sudden loading, sending intense pain that sometimes shoots down the leg immediately.
The third, and most serious, is cauda equina syndrome. This is a medical emergency where the spinal nerve bundle is suddenly. It causes back pain plus loss of bladder or bowel control, numbness in the inner thighs, and weakness in both legs. This requires emergency surgery within hours to prevent permanent nerve damage.
What Are Signs of Serious Back Pain During Pregnancy?
Most pregnancy back pain is normal. The uterus shifts the center of gravity, hormones loosen ligaments, and the lower back compensates by arching more. That causes aching. It’s uncomfortable but not dangerous.
The warning signs that need immediate medical attention are:
- Back pain with rhythmic cramping or contractions before 37 weeks (possible preterm labor)
- Sudden severe pain in the upper back or between shoulder blades (can indicate preeclampsia)
- Back pain with vaginal bleeding
- Pain with burning urination (kidney infection during pregnancy progresses fast and risks preterm birth)
- Numbness or weakness that spreads to the legs
Pain that stays only in the lower back, worsens at the end of the day, and improves with rest is typical pregnancy strain. The pattern matters.
How to Sleep With Pregnancy Back Pain?
The position that takes the most pressure off a pregnant back is side-lying with a pillow between the knees. The left side is better for circulation.
A full-length pregnancy pillow (like a C-shaped or U-shaped body pillow) supports the belly and stops the spine from rotating. Placing a small pillow under the belly while side-lying also reduces strain on the lumbar spine.
Avoid sleeping flat on your back after the second trimester. The uterus compresses the vena cava (the major vein returning blood to the heart), which reduces circulation and increases back pressure. A firm mattress makes a measurable difference compared to a sagging one.
What’s the Best Treatment for Back Pain?
For acute (short-term) back pain lasting under 4 weeks, the evidence strongly supports:
- Staying active. Bed rest slows recovery. Gentle movement keeps muscles from tightening further.
- NSAIDs (ibuprofen, naproxen): More effective than acetaminophen for back pain according to a 2017 Annals of Internal Medicine analysis.
- Heat therapy: Applied 20 minutes at a time reduces muscle spasm and increases blood flow.
For chronic back pain (lasting over 3 months), physical therapy focused on strengthening the core and improving posture outperforms medication in the long term. Cognitive Behavioral Therapy (CBT) also works for chronic pain because it changes how the brain processes pain signals.
How to Cure Back Pain Naturally?
Natural approaches with solid clinical backing:
- Core strengthening exercises (specifically the McGill Big 3, covered below) reduce recurring back pain better than general exercise
- Yoga: A 2017 study in Annals of Internal Medicine found yoga produced similar results to physical therapy for chronic lower back pain
- Massage therapy: Reduces muscle tension and pain for up to 6 weeks per treatment course
- Acupuncture: Multiple reviews confirm it reduces chronic back pain better than sham acupuncture and better than some medications
- Topical arnica gel: Reduces localized muscle pain with fewer GI side effects than oral NSAIDs
None of these replace physical therapy for structural problems like disc herniation. For muscle-based or postural back pain, they work well.
How to Make Lower Back Pain Go Away?
For pain that showed up in the last few days:
- Apply heat for 20 minutes, 3 times daily (ice works better in the first 48 hours right after injury)
- Take ibuprofen 400 mg with food every 6 to 8 hours for up to 5 days
- Keep moving with light walking, even if it’s uncomfortable
- Avoid sitting for more than 30 minutes without standing up and moving
What Can Be Done for Long-Term Back Pain?
Chronic back pain (more than 3 months) needs a different approach than acute pain.
- Physical therapy with a specific focus on motor control and posture correction is the most effective long-term solution
- Pain neuroscience education: Learning how chronic pain works in the brain actually reduces pain intensity. This isn’t about mindset, it’s about reteaching the nervous system.
- Low-dose naltrexone (LDN): An emerging option that reduces neuroinflammation. Some pain clinics now prescribe it for chronic spine pain.
- Spinal cord stimulation: An implanted device that interrupts pain signals before they reach the brain. Used for people who haven’t responded to other treatments.
- Mindfulness-Based Stress Reduction (MBSR): A 2016 JAMA Internal Medicine study found it produced significantly better outcomes for chronic back pain than standard medical care alone
Surgery is rarely the answer for chronic back pain without a clear structural cause. About 40% of spinal fusion surgeries don’t provide significant long-term pain relief.
Which Vitamins Reduce Back Pain?
Four nutrients directly affect back pain:
- Vitamin D: Low vitamin D causes bone and muscle aching, including in the back. A 2008 study found that 83% of chronic back pain patients were vitamin D deficient. Supplementing at 2,000 to 4,000 IU daily corrects this.
- Magnesium: Deficiency causes muscle tension and spasm. Magnesium glycinate at 300 to 400 mg daily relaxes muscles including those along the spine.
- Vitamin B12: Deficiency causes nerve pain and sometimes presents as back pain, especially in older adults.
- Omega-3 fatty acids (fish oil): Reduces disc inflammation. A University of Pittsburgh study found fish oil supplementation reduced spinal pain as effectively as ibuprofen in a significant percentage of patients.
Is Walking Good for Back Pain?
Yes, walking is one of the best things for most types of back pain. It activates back muscles without overloading the spine, increases blood flow to disc tissue (which has poor circulation), and releases endorphins that reduce pain perception naturally.
A 2019 study in the European Spine Journal confirmed that walking programs reduced chronic low back pain and disability as effectively as specific exercise therapy.
The right amount: 20 to 30 minutes at a moderate pace, most days. Flat surfaces work better than hills in the early stages. Stop if pain exceeds a 4 out of 10 during the walk.
Can Back Pain Be Cured Without Surgery?
For the vast majority of back pain cases, yes. About 90% of acute back pain resolves within 6 weeks without surgery. Even disc herniations, which people often assume need surgical repair, resolve without surgery in about 70% of cases within 6 to 12 weeks.
Surgery is genuinely necessary when there’s nerve compression causing progressive weakness, when cauda equina syndrome is present, or when structural problems cause severe functional loss and don’t respond to 6 months of proper conservative treatment.
For chronic pain without clear structural damage, surgery shows poor outcomes. Physical therapy, exercise, and pain management work better and carry zero surgical risk.
What Is the Big 3 for Back Pain?
The “Big 3” is a spine rehabilitation protocol developed by Dr. Stuart McGill, a spinal biomechanics professor at the University of Waterloo.
The three exercises are:
- The McGill Curl-Up Lie on your back with one knee bent. Place your hands under your lower back to maintain its natural curve. Lift only your head and shoulders slightly off the ground. Hold 8 to 10 seconds. This trains the abdominal wall without flexing the lumbar spine.
- The Bird-Dog Get on all fours. Extend one arm forward and the opposite leg back simultaneously. Keep the back flat. Hold 8 to 10 seconds. Switch sides. This builds deep spinal stabilizer muscles.
- The Side Plank Lie on your side, propped on one elbow. Lift your hips off the ground, forming a straight line. Hold 8 to 10 seconds. This trains the quadratus lumborum, the deep lateral muscle that most back pain programs completely ignore.
McGill recommends 3 sets of 6 repetitions for each, done daily. Multiple studies confirm this combination reduces back pain and prevents recurrence better than generic core exercises like standard crunches or sit-ups, which actually increase disc pressure.











Leave a Comment