Polyps cause constipation in some people, though not everyone with polyps experiences this symptom. These small growths inside your colon can partially block the passage where stool moves through, making it harder to have regular bowel movements.
Constipation happens when polyps grow large enough or appear in certain locations that interfere with normal digestion. While many polyps stay small, bigger polyps or clusters of polyps can cause constipation.
If you have colon polyps, you feel nothing at all. That’s why doctors recommend screenings after age 45. But when polyps cause constipation, stools get thinner, requiring you to strain more than usual or making you feel like you can’t fully empty your bowels.
Constipation Due to Colon Polyps
Constipation due to colon polyps develops through physical and functional changes in your digestive system. The polyp growths can interfere with the normal rhythm and flow of waste material moving toward your rectum.
How Colon Polyps Affect Stool Movement
When a polyp grows on the colon wall, it takes up space that stool needs to pass through. This creates partial narrowing of the space (bowel lumen).
Polyps can disrupt bowel movement, causing altered intestinal motility. This irregular movement pattern causes stool to sit in your colon longer than it should, which makes it drier and harder to pass.
When Polyps Are More Likely to Cause Constipation
Larger polyps (usually over 1 centimeter, about the size of a pea) are more likely to create blockage issues.
Multiple polyps increase the chances that polyps cause constipation. Even if each growth is relatively small, having several scattered throughout your colon causes constipation.
Polyps in the distal colon (the last section before your rectum) or directly in the rectum itself cause more problems. The rectum is narrower, so growths here block more of the available space.
Can Polyps Change Bowel Habits?
Yes, polyps can change bowel habits. Bowel habit changes often appear gradually and might seem minor at first.
Types of Bowel Changes Seen
New-onset constipation: You suddenly need to strain during bowel movements when this was never an issue before. Where you once passed stool daily without thinking about it, you now go every few days or struggle each time.
Alternating constipation and diarrhea: One week you can’t pass stool, the next week you have loose stools. This happens because the polyp partially blocks the colon, and liquid stool can sometimes squeeze past, while formed stool cannot.
A feeling of incomplete evacuation: You finish using the bathroom, but still feel full. You know more stool should come out, but you can’t make it happen. This sensation relates to polyps near the rectum that make the area feel occupied even after you’ve emptied what you can.
How These Changes Differ From Functional Constipation
Regular constipation (the kind from not drinking enough water or eating enough fiber) usually responds when you drink more fluids, eat prunes, add vegetables, and maybe take a fiber supplement. Constipation due to colon polyps shows a progressive pattern. It gets worse over time.
Laxatives might help temporarily when polyps cause constipation, but the relief doesn’t last. When laxatives show poor response despite good compliance, physical blockage becomes more likely than simple slow digestion.
Constipation and Colon Polyps Symptoms

Constipation and colon polyps symptoms often appear as a cluster rather than one isolated problem.
Symptoms That May Occur Together
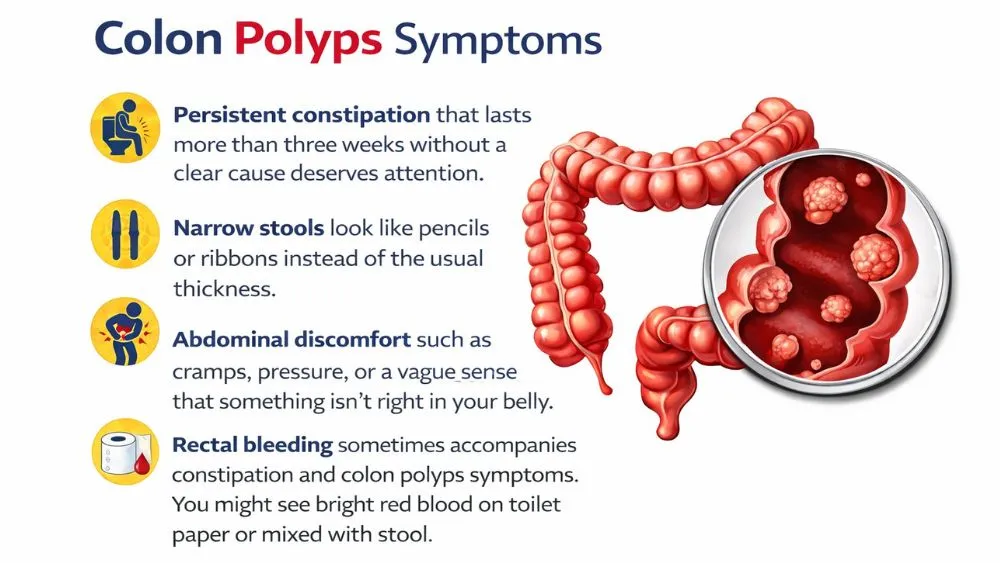
- Persistent constipation that lasts more than three weeks without a clear cause deserves attention.
- Narrow stools look like pencils or ribbons instead of the usual thickness.
- Abdominal discomfort such as cramps, pressure, or a vague sense that something isn’t right in your belly.
- Rectal bleeding sometimes accompanies constipation and colon polyps symptoms. You might see bright red blood on toilet paper or mixed with stool.
Red-Flag Symptoms
Unexplained weight loss combined with constipation raises serious concern. Losing 10 pounds or more without trying, especially when paired with bowel changes, needs immediate medical attention.
Iron-deficiency anemia shows up in blood tests as low red blood cell counts and low iron levels. This happens when polyps bleed slowly over time.
Blood mixed with stool (not just on the surface) looks dark or makes stool appear black and tarry. This indicates bleeding higher up in your digestive tract.
Can Colon Polyps Block Stool?
Yes, colon polyps can block stool depends on several factors, but complete blockage from polyps alone is uncommon.
Partial vs Complete Blockage
Most polyps cause partial obstruction only. You still have bowel movements, just less frequently or with more difficulty. Stool can squeeze past the growth, though not as easily as it should.
Complete blockage is rare with typical polyps. It usually requires either a very large polyp in a narrow section of the colon or a cancerous growth that’s been expanding for a long time.
Symptoms of Concerning Obstruction
Severe constipation that progresses to no bowel movements for several days signals a possible serious blockage. You feel the urge, but nothing comes out, no matter what you try.
Abdominal pain and bloating get progressively worse. Your belly swells, becomes hard to touch, and hurts constantly rather than coming and going.
Vomiting or inability to pass gas indicates advanced obstruction. Not being able to pass even gas means the blockage is total. These symptoms constitute a medical emergency requiring hospital care.
Intestinal Polyps Constipation: Who Is at Higher Risk
Intestinal polyps and constipation affect people aged 45 to 50, substantially increasing risk. This is why screening colonoscopies typically start at age 45 for people with average risk.
Family history of polyps or colon cancer multiplies your risk. If your parents, siblings, or children have had polyps or colon cancer, your chances increase significantly.
History of inflammatory bowel disease (like Crohn’s disease or ulcerative colitis) raises risk for both polyps and cancer.
Long-standing unexplained constipation without clear cause warrants investigation, especially after age 40.
How Constipation Related to Polyps Is Diagnosed
Doctors use several approaches to determine if polyps cause constipation in your specific case.
Your doctor will ask when constipation started, how it has changed, what you’ve tried, and what other symptoms accompany it. This conversation helps distinguish polyp-related constipation from other causes.
Stool tests check for hidden blood that you can’t see. If bleeding is suspected, these tests can detect tiny amounts.
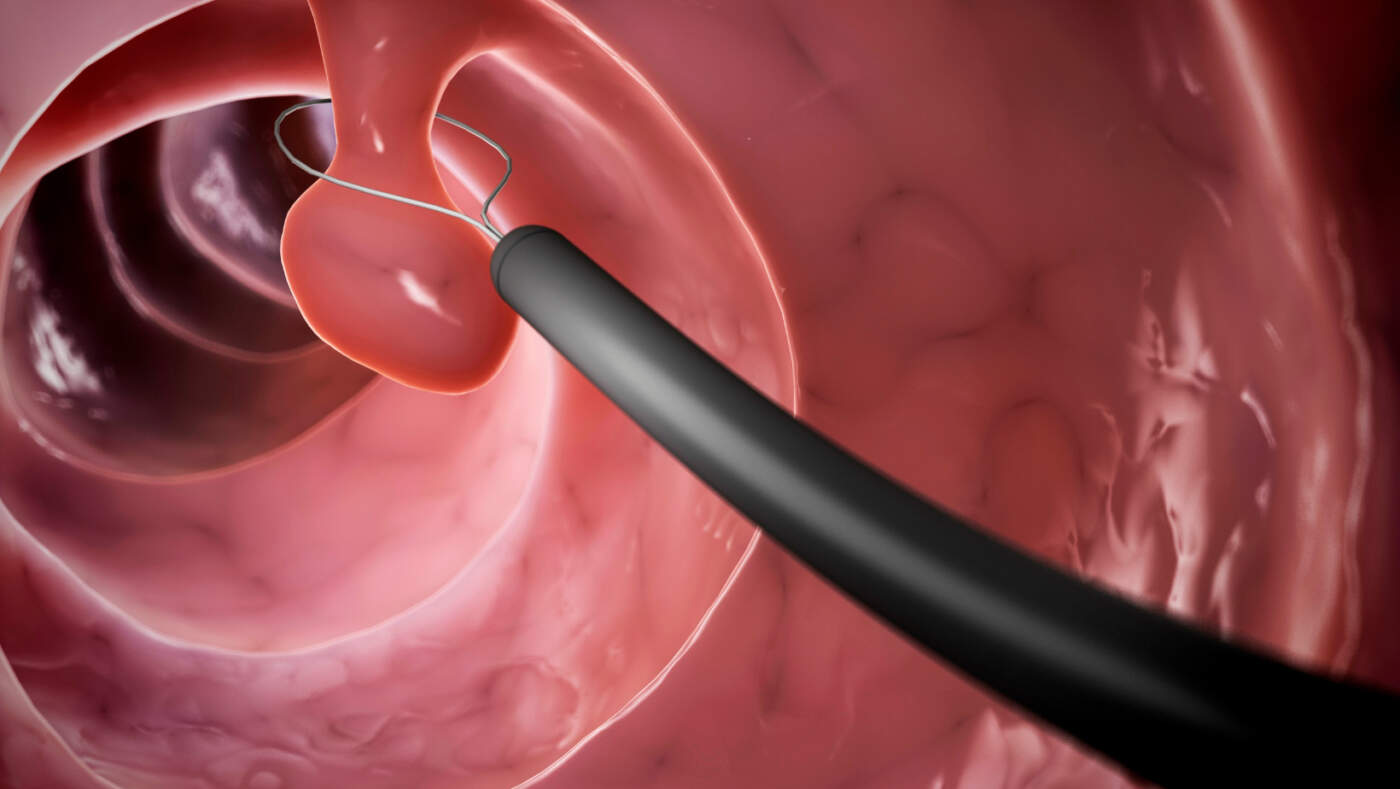
Colonoscopy serves is the definitive test to see polyps directly. If found, polyps can be removed during the same procedure. While the preparation and procedure itself require planning, colonoscopy remains the gold standard for both finding and treating polyps.
Treatment When Polyps Cause Constipation
Polyp removal resolves symptoms in most cases. Once the physical obstruction disappears, normal bowel function typically returns within days to weeks.
Constipation management is supportive until removal. Your doctor might recommend stool softeners or mild laxatives to keep you comfortable while waiting for your colonoscopy appointment.
Avoid masking symptoms with long-term laxatives. What starts as manageable constipation could worsen over time if the polyps aren’t removed.
When to See a Doctor for Constipation and Suspected Polyps
Constipation lasting more than three weeks without explanation deserves medical evaluation. Brief episodes happen to everyone, but persistent problems need investigation.
A change in bowel habits after age 45 should prompt a conversation with your doctor. Constipation with blood or anemia signals possible polyps, inflammation, or other conditions needing diagnosis.
Constipation not responding to standard treatment (increased fiber, fluids, exercise, over-the-counter remedies) within a reasonable timeframe needs medical evaluation.
FAQs on Polyps and Constipation
Can polyps really cause constipation?
Yes. Large polyps or multiple smaller ones can narrow your colon enough to slow stool movement. The blockage is usually partial, making bowel movements difficult but not impossible. Location matters too since polyps near your rectum create more symptoms than those higher up.
Do most colon polyps cause symptoms?
No. Most polyps stay small and produce zero symptoms. You could have several polyps and never know without a screening test. Only about 5% of polyps grow large enough or are positioned where they create noticeable problems like constipation or bleeding.
Can polyps change bowel habits suddenly?
Not typically. Polyps changing bowel habits gradually is more accurate. The changes develop over weeks or months as polyps grow. Sudden dramatic changes in one or two days usually point to infections, food reactions, or medication effects rather than polyps.
Is constipation a common sign of colon polyps?
It’s uncommon but possible. Most people with polyps experience no symptoms at all. When symptoms do appear, bleeding is more common than constipation. Constipation from polyps usually means you have larger growths or multiple polyps affecting how your colon works.
Can polyps cause narrow stools?
Yes. When a polyp grows large enough to take up significant space in your colon, stool must squeeze past it. This compression makes stools thinner, like pressing play dough through a smaller opening. Consistently narrow stools warrant medical evaluation.
Can laxatives fix constipation caused by polyps?
Only temporarily. Laxatives might soften stool enough to pass the blockage, providing short-term relief. But the polyp remains, so constipation returns. Laxatives treat the symptom but not the cause. Removing the polyp fixes the actual problem.
Is constipation from polyps painful?
Sometimes. You might feel cramping, pressure, or discomfort when stool builds up behind the polyp. The straining needed to pass stool can also cause pain. However, many people with polyps cause constipation experience only mild discomfort rather than severe pain.
Can intestinal polyps cause bloating and gas?
Yes. When intestinal polyps cause constipation slows digestion, waste sits in your colon longer. This gives bacteria more time to produce gas, leading to bloating. The partial blockage can also trap gas, making you feel distended and uncomfortable.
Does removing polyps improve constipation?
Usually. You notice improvement within days to weeks after polyp removal. Your colon needs time to return to normal function, but once the physical obstruction is gone, constipation typically resolves. Some people need temporary fiber supplements during recovery.
When should constipation raise concern for polyps?
After age 45 with new constipation, when it lasts over three weeks, if you see blood, or when standard treatments fail. Also worry if constipation comes with weight loss, anemia, or dramatically narrower stools. These combinations justify seeing a doctor soon.











Leave a Comment