Yes, kidney stones can cause diarrhea more often than you expect. Kidney stones are painful enough on their own. Adding diarrhea, cramping, and gut urgency makes a bad situation harder. The pain is severe with nervous system responses, and medications used during a kidney stone attack all trigger loose stools or diarrhea.
If you’re in the middle of a stone attack, focus on fluids and pain control. If GI symptoms outlast the stone, seek emergency care immediately.
Kidney Stones and Diarrhea Symptoms
Classic Kidney Stone Symptoms
Kidney stones don’t always cause symptoms. When they do, it’s usually because the stone is moving.
The most common symptoms include:
- Severe flank pain: A stabbing or cramping pain in the lower back or side, just below the ribs. It comes in waves and gets worse fast.
- Radiating pain to the groin: As the stone moves down the ureter, pain shifts toward the lower abdomen and groin. Men sometimes feel it in the testicles.
- Nausea and vomiting: The pain is intense enough to trigger the body’s nausea response. You will vomit at least once during a bad stone attack.
Possible GI Symptoms
Kidney stones and diarrhea symptoms often appear together because the kidneys and intestines share a nerve pathway.
GI symptoms during a kidney stone episode include:
- Diarrhea: Loose or watery stools during or shortly after intense flank pain
- Abdominal cramping: Spasms in the lower belly that feel similar to food poisoning
- Urgency: A sudden, pressing need to use the bathroom with little warning
These symptoms don’t mean the stone has moved into your intestines. That’s not how kidney stones work. The gut is reacting to the pain and stress signals the body is sending.
Diarrhea During a Kidney Stone Attack
Stress and Autonomic Nervous System Activation
When you’re in severe pain, your autonomic nervous system, the part of the nervous system that controls involuntary functions, triggers a fight-or-flight response. Heart rate spikes, muscles tense, and the bowels speed up.
This is called autonomic dysregulation. Kidney stone pain ranks among the most severe pains a human body experiences, right alongside childbirth and burns. The body reacts accordingly.
Intense ureteral spasms send pain signals that cross over into gut nerve pathways, producing cramping and urgency in the intestines.
Medication-Related Effects
The medications given during a kidney stone attack also contribute.
NSAIDs (like ibuprofen or ketorolac): These are first-line pain treatments for kidney stones. NSAIDs irritate the gut lining. High doses, which are often needed for stone pain, commonly cause loose stools, stomach cramping, and diarrhea, especially on an empty stomach.
Antibiotics (if infection is present): Sometimes, kidney stones cause a secondary UTI or kidney infection. Antibiotics fluoroquinolones, trimethoprim-sulfamethoxazole, or nitrofurantoin are well-known for disrupting gut bacteria and causing diarrhea. Fluoroquinolones in particular carry a higher risk of Clostridioides difficile overgrowth, which causes severe diarrhea.
Types of Kidney Stones Associated with Bowel Disease
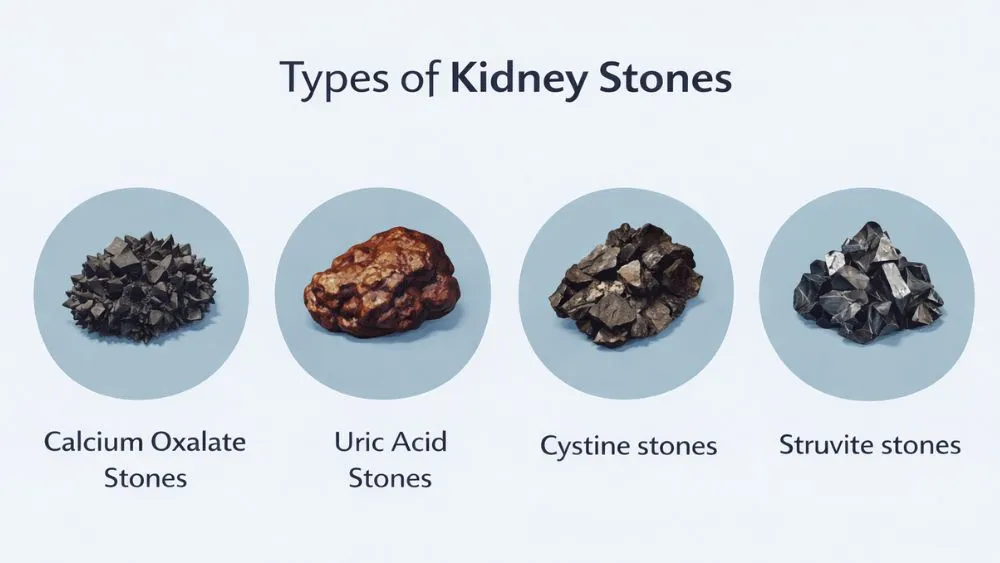
Calcium Oxalate Stones
Calcium oxalate stones are the most common type overall. They’re also heavily linked to inflammatory bowel disease (IBD), specifically Crohn’s disease.
In IBD, the small intestine absorbs fat poorly. Unabsorbed fat binds to calcium in the gut. This leaves oxalate free to be absorbed into the bloodstream in large amounts. The kidneys then excrete this excess oxalate, and it crystallizes with calcium in the urine, forming stones.
Uric Acid Stones
Uric acid stones form in acidic urine. They’re directly linked to conditions that cause chronic diarrhea. Chronic diarrhea leads to dehydration and loss of bicarbonate in stool. This makes urine more acidic. Uric acid doesn’t dissolve well in acidic urine; it crystallizes.
These types of kidney stones associated with bowel disease are also harder to spot on standard X-rays because they’re radiolucent. CT scans catch them.
Treating Diarrhea as a Kidney Stone Passes
Treating diarrhea as a kidney stone passes requires addressing the stone and the gut symptoms. They’re related, so managing one helps the other.
Hydration Strategy
Dehydration concentrates urine, slows stone passage, and makes diarrhea harder on the body.
- Oral fluids: Aim for 2–3 liters per day if tolerated. Water is best. Avoid caffeine and alcohol: both worsen dehydration.
- Electrolytes: Diarrhea depletes sodium and potassium fast. Oral rehydration solutions (ORS) like Pedialyte restore electrolyte balance better than plain water. Sports drinks work in a pinch but contain sugar that sometimes worsens diarrhea.
If vomiting prevents oral intake, IV fluids in an ER are necessary.
Pain Control
Proper pain control actually reduces GI symptoms, and the bowel urgency often eases.
Doctors typically use:
- Ketorolac (IV NSAID) for acute attacks
- Alpha-blockers like tamsulosin relax the ureter and help the stone pass faster
- Opioids, in severe cases, though these slow the gut and sometimes cause constipation once diarrhea resolves
Diet During Recovery
Eat light because gut is already irritated.
- Stick to bland foods: plain rice, toast, bananas, boiled potatoes
- Avoid high-oxalate foods (spinach, nuts, beets) if you have calcium oxalate stones
- Skip spicy foods, dairy, and anything high-fat until diarrhea fully resolves
- Probiotic foods like plain yogurt help restore gut bacteria disrupted by antibiotics
When Diarrhea Is NOT From Kidney Stones
Kidney stones that cause diarrhea do not last weeks. If diarrhea persists beyond the stone-passing period, something else is causing it.
Watch for these signs that diarrhea has a different source:
- Persistent diarrhea with no flank pain: Kidney stone diarrhea follows the pain. If there’s no pain, there’s no stone driving it.
- Fever and blood in stool: This points to intestinal infection, colitis, or IBD, not kidney stones.
- Chronic bowel habit change: A shift in your normal bowel pattern lasting more than 3–4 weeks warrants a colonoscopy, not kidney stone treatment.
When to Seek Medical Care
Go to the ER if you have:
- Fever with stone symptoms: This combination signals a kidney infection (pyelonephritis), which can become life-threatening within hours without antibiotics.
- Severe dehydration: Signs include no urination for 8+ hours, extreme dizziness, and dry mouth despite drinking fluids.
- Inability to pass urine: If a stone blocks urine flow completely, pressure builds in the kidney. This is a urologic emergency.
- Persistent vomiting: If you can’t keep fluids down, you need IV hydration and IV pain management.
FAQs on Kidney Stones and Diarrhea
Is diarrhea a common kidney stone symptom?
Yes, 30% of kidney stone patients have GI symptoms, including diarrhea. It’s driven by autonomic nervous system activation from intense pain. It’s not in the stone itself causing it; it’s the body’s pain response.
Can a kidney stone irritate the intestines?
Not directly. Kidney stones stay in the urinary tract; they never enter the intestines. But the ureter runs close to bowel nerve pathways. When the ureter spasms around a stone, those spasms send pain signals that trigger intestinal cramping and urgency via shared nerve networks.
Does severe pain trigger diarrhea?
Yes. Extreme pain activates the sympathetic nervous system, which can speed up bowel motility. Kidney stones cause diarrhea as a documented stress response. The pain of a kidney stone is severe enough to trigger this in many patients.
Can dehydration from stones cause bowel changes?
Yes. Dehydration typically slows the gut and causes constipation. But combined with nervous system activation and nausea, the net result varies. Some patients get constipation; others get diarrhea. If diarrhea is severe, it worsens the dehydration the stone already caused.
Are antibiotics for stones linked to diarrhea?
Yes. Fluoroquinolones prescribed for stone-related infections disrupt gut flora within 48 hours. Around 10–25% of patients on antibiotics develop antibiotic-associated diarrhea. Taking a probiotic alongside the antibiotic reduces this risk.
Can chronic diarrhea increase kidney stone risk?
Yes. Chronic diarrhea causes bicarbonate loss, which acidifies urine. Acidic urine promotes uric acid stone formation. It also dehydrates the body, concentrating minerals that form types of kidney stones associated with bowel disease, like calcium oxalate and uric acid stones.
Is diarrhea during a stone attack dangerous?
Rarely, on its own. The danger is dehydration. If diarrhea is severe and you’re also vomiting, you lose fluids fast. Combined with the fact that kidney stone pain makes eating or drinking difficult, dehydration can escalate quickly and require IV fluids.
Should I treat diarrhea separately from the stone?
Focus on hydration and electrolyte replacement: that helps both. Treating the pain properly also reduces autonomic-driven diarrhea. Avoid anti-diarrheal medications like loperamide without doctor clearance, especially if infection is suspected.
Does passing a stone stop diarrhea?
Usually yes. Once the stone passes and pain resolves, the autonomic nervous system calms down. Most patients see GI symptoms resolve within 12–24 hours of passing the stone. If diarrhea continues beyond 48 hours after the stone passes, see a doctor.
When should I worry?
Worry when diarrhea comes with fever above 38.5°C (101.3°F), no urination for 8+ hours, or blood in stool. These are not normal kidney stone symptoms, and need medical attention.














Leave a Comment