A nursing diagnosis for urinary tract infection is a formal clinical statement nurses use to identify a patient’s specific problems related to a UTI, so they can build the right care plan. UTIs affect around 150 million people globally each year.
Women are the most affected group, though older adults and people with catheters face high risk too. This guide covers the priority diagnoses, risk factors, nursing interventions, patient education, and complications nurses watch for when caring for UTI patients.
Priority Nursing Diagnosis for UTI
The priority nursing diagnosis for UTI covers problems that need immediate attention. Nurses rank these by how directly they affect the patient’s safety and comfort.
Impaired Urinary Elimination UTI Diagnosis
Impaired urinary elimination UTI diagnosis is almost always the top priority. It means the patient has trouble urinating normally because the infection has inflamed the bladder and urethra (the tube that carries urine out). Symptoms include painful urination, urgency (sudden strong need to go), and frequency (going very often, even at night). Left unmanaged, this increases the risk of urine backing up toward the kidneys.
Acute Pain Related to Inflammation
Pain is a top-priority concern in any nursing diagnosis for urinary tract infection. The infection inflames the bladder lining, causing a burning sensation while urinating and cramping in the lower abdomen. Nurses use a pain scale (0 to 10) to measure severity and track changes after treatment begins. Managing pain also keeps patients willing to drink fluids, which speeds recovery.
Risk for Infection Spread
A UTI that is not treated quickly can spread from the bladder to the kidneys or enter the bloodstream. This risk shapes the priority nursing diagnosis for UTI list. Nurses monitor temperature, heart rate, and urine color for signs of spreading infection. Fever above 101°F (38.3°C), chills, and kidney-area back pain are the main warning signs.
Other Common Nursing Diagnoses for UTI
Acute Pain
Pain from a UTI goes beyond urination. Patients feel pelvic pressure and constant cramping. Nurses document this separately from urinary elimination because it needs its own management plan, including prescribed pain relievers and a warm compress on the lower abdomen.
Risk for Sepsis (in Severe Cases)
Sepsis is rare but possible, especially in older adults or patients with weakened immune systems. When a UTI reaches the bloodstream, it becomes a medical emergency. A nursing diagnosis for urinary tract infection that includes sepsis risk means nurses must monitor blood pressure, breathing rate, and mental alertness closely.
Deficient Knowledge (Patient Education)
Many patients do not know what causes UTIs or how to prevent recurrence. In nursing care, this is formally labeled a deficient knowledge diagnosis. The nurse is responsible for educating the patient about hygiene, hydration, and completing antibiotics. Without this, UTI recurrence stays high. Up to 25 percent of women have a repeat UTI within 6 months.
Risk for Fluid Volume Deficit
Patients with UTIs often avoid drinking water because urination is painful. This leads to dehydration, which concentrates urine and worsens the infection. Nurses track fluid intake and output and encourage steady hydration.
Risk Factors for UTI Nursing Diagnosis
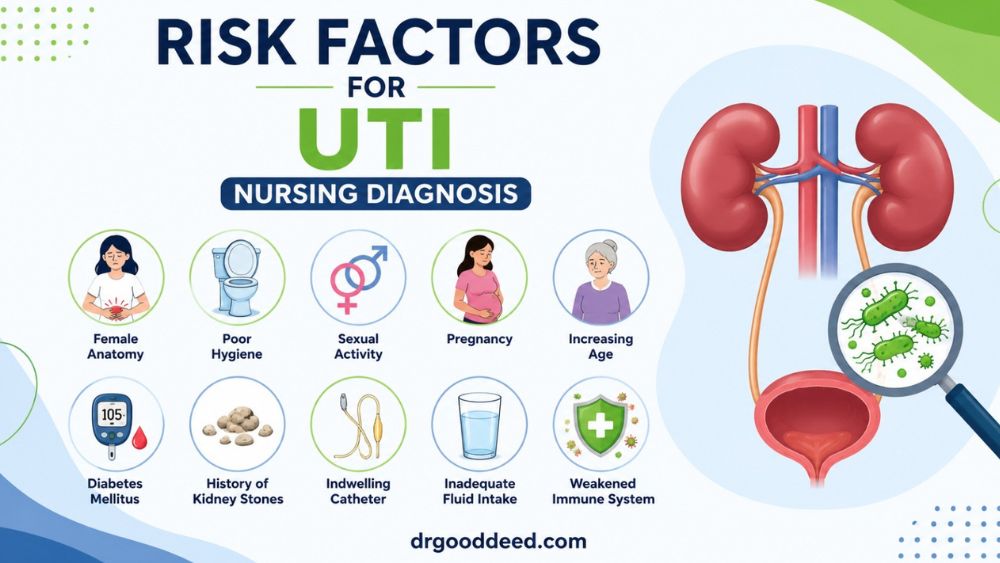
Understanding risk factors for UTI nursing diagnosis helps nurses identify which patients need the most attention and preventive care.
Poor Hygiene and UTI Risk Nursing
Poor sleep hygiene and UTI risk go hand in hand in nursing. Bacteria from the skin or stool can enter the urethra if the genital area is not cleaned properly. Wiping back to front after using the toilet is one of the most common causes of bacterial entry. Nurses identify poor hygiene as a modifiable risk, meaning the patient can change it with education.
Urinary Retention
When the bladder does not empty fully, leftover urine becomes a breeding ground for bacteria. An enlarged prostate (in men), nerve damage (neurogenic bladder), or certain medications can cause retention. Nurses check post-void residual volume (how much urine stays after urinating) using ultrasound or a catheter.
Catheter Use
Urinary catheters are one of the leading causes of hospital-acquired UTIs, called CAUTIs (catheter-associated urinary tract infections). The risk factors for UTI nursing diagnosis in catheterized patients include insertion technique, catheter duration, and drainage bag management. Nurses use strict sterile technique to reduce this risk.
Female Anatomy and Age Factors
Women have a shorter urethra than men, giving bacteria a shorter path to the bladder. This is a major risk factors for UTI nursing diagnosis consideration. Postmenopausal women have lower estrogen, which thins the urinary tract lining and reduces natural bacterial defenses. Elderly patients of both sexes face higher risk due to weaker immune systems.
Assessment Data for UTI (Nursing Evaluation)
Before forming any nursing diagnosis for urinary tract infection, nurses collect both subjective and objective data.
Subjective data is what the patient reports. Common complaints include:
- Burning or stinging while urinating
- Sudden, strong urge to urinate
- Feeling like the bladder never fully empties
- Lower abdominal pressure
- Foul-smelling urine
Objective Data (Fever, Cloudy Urine, Lab Results)
Objective data is what the nurse measures directly. This includes:
- Fever (above 99.5°F or 37.5°C)
- Cloudy or dark urine
- Elevated white blood cell count on blood tests
- Bacteria in urine culture
- Tenderness when pressing on the lower abdomen
Urinalysis Findings
A urinalysis is the most important diagnostic tool for UTIs. Key findings include:
- Positive nitrites (sign that certain bacteria are present)
- High leukocyte esterase (marker for white blood cells in urine)
- Bacteria visible under a microscope
- pH above 7 (more alkaline than normal)
A urine culture then identifies the exact bacteria and which antibiotic works best.
Nursing Interventions for UTI Care Plan
Nursing interventions for UTI care plan are the specific actions nurses take to help the patient recover and prevent complications.
Monitoring Urinary Patterns
Nurses document how often the patient urinates, how much comes out each time, and whether pain changes. This tracking measures whether treatment is working.
Encouraging Fluid Intake
Increasing fluid intake flushes bacteria out of the bladder. Nurses aim for 2 to 3 liters of water daily unless a heart or kidney condition limits fluid. Patients should cut out caffeine and alcohol, as both irritate the bladder lining.
Administering Prescribed Antibiotics
Antibiotics are the main treatment for UTIs. Dosage varies by age, kidney function, and the bacteria identified. Nurses give medications on time, watch for adverse reactions like rashes or stomach upset, and reinforce that stopping antibiotics early allows resistant bacteria to return.
Promoting Hygiene Practices
Nurses teach proper perineal (genital area) care, including front-to-back wiping, gentle cleansing with warm water, and avoiding scented soaps near the urethra. This is a core part of nursing interventions for UTI care plan because it directly reduces the chance of reinfection.
Patient education is a formal part of any nursing diagnosis for urinary tract infection care plan. Without it, recurrence rates stay high.
Proper Hygiene Techniques
Teach patients to wipe front to back after every bathroom trip. Use mild, unscented soap for the external genital area. Avoid douching, as it disrupts the natural bacterial balance and increases UTI risk.
Completing Antibiotic Course
Patients must finish the full antibiotic course: typically 3 to 7 days for uncomplicated UTIs and up to 14 days for kidney infections. Stopping early is one of the top reasons UTIs come back, even when the patient feels better.
Preventing Recurrence
Practical prevention tips nurses should share:
- Urinate after sexual activity to flush bacteria from the urethra
- Drink enough water daily (pale yellow urine is the goal)
- Avoid holding urine for long periods
- Wear breathable cotton underwear
- For women with frequent UTIs, ask a doctor about a low-dose preventive antibiotic
Every nursing diagnosis for urinary tract infection care plan must include a watchlist for these complications, especially in high-risk patients.
Kidney Infection (Pyelonephritis)
Pyelonephritis (kidney infection) happens when bladder bacteria travel up to the kidneys. Signs include high fever, shaking chills, flank pain (side-of-body pain near the kidneys), nausea, and vomiting. Severe cases require IV (intravenous, directly into the vein) antibiotics and hospital admission.
Sepsis
Sepsis from a UTI is a medical emergency. Nurses monitor for rapid heartbeat (above 90 beats per minute), low blood pressure (below 90/60 mmHg), confusion, and fast breathing. A nursing diagnosis for urinary tract infection in elderly patients must always include sepsis risk on the watchlist.
Recurrent Infections
Three or more UTIs in one year is considered recurrent. Nurses flag this pattern and ensure the doctor is aware. Recurrent cases need further investigation for anatomical issues, diabetes, or immune deficiency.
FAQs
What Is a Nursing Diagnosis for Urinary Tract Infection?
A nursing diagnosis for urinary tract infection is a clinical statement nurses use to describe a patient’s specific UTI-related problem. Examples include impaired urinary elimination, acute pain, and risk for sepsis. It guides the care plan. It is different from a medical diagnosis, which is made by a doctor.
What Is Impaired Urinary Elimination UTI Diagnosis?
Impaired urinary elimination UTI diagnosis means the patient cannot urinate normally due to bladder inflammation from infection. Signs include burning, urgency, frequency, and incomplete emptying. It is typically the first nursing diagnosis assigned because it directly affects comfort, hydration, and infection control.
How Does Poor Hygiene Increase UTI Risk?
Poor hygiene and UTI risk nursing are directly linked. Wiping back to front moves bowel bacteria (mainly E. coli) toward the urethra. Studies show E. coli causes 80 to 85 percent of all UTIs. Teaching correct wiping technique and daily perineal care reduces recurrence measurably.
What Are Nursing Interventions for UTI Care Plans?
Nursing interventions for UTI care plan include monitoring urinary frequency and output, pushing 2 to 3 liters of daily fluid intake, giving antibiotics on schedule, tracking pain levels using a 0 to 10 scale, and teaching front-to-back hygiene. These steps together address both infection clearance and symptom relief.
What Are Goals for UTI Nursing Care?
Goals include pain reduction to a 2 or below on the pain scale within 48 hours of antibiotic start, clear urine within 3 to 5 days, no fever, normal urinary frequency, and patient ability to correctly explain prevention steps before discharge. These are measurable, time-bound targets.
How to Evaluate UTI Nursing Interventions?
Nurses evaluate success by checking: urine clarity, pain scores, urination frequency, temperature, lab results, and whether the patient can name at least three UTI prevention steps. If symptoms worsen after 48 hours of antibiotics, the care team reassesses the antibiotic choice based on culture results.
How to Educate Patients About UTI Prevention?
Teach patients three non-negotiable habits: drink at least 2 liters of water daily, urinate within 15 minutes of sexual activity, and wipe front to back every time. For women with three or more UTIs per year, ask the doctor about post-coital (after-sex) antibiotic prophylaxis (a single preventive dose). These steps cut recurrence risk significantly.