A peptic ulcer is an open sore that forms on the inner lining of your stomach or the upper part of your small intestine. Natural remedies for peptic ulcer can reduce pain, protect the stomach lining, and support healing.
Most peptic ulcers form because of two reasons: H. pylori bacterial infection or long-term use of NSAIDs like ibuprofen or aspirin. Both need medical treatment.
Peptic ulcer recovery depends on treating the cause first. H. pylori needs antibiotics. NSAID damage needs stopping the drug. Natural remedies for peptic ulcer build on that foundation.
Cabbage juice, DGL, probiotics, and raw honey all have real evidence behind them. A clean diet, stress management, and zero alcohol make measurable differences in healing time.
Can Peptic Ulcers Be Treated Naturally?
Natural remedies for peptic ulcer reduce inflammation, protect the stomach wall, and ease symptoms like burning and bloating. They do not eliminate H. pylori on their own. They do not reverse damage from NSAIDs alone.
H. pylori bacteria affect roughly 44% of the global population. In India, prevalence is even higher, around 58 to 68% in some studies. If your ulcer comes from H. pylori, you need a “triple therapy” antibiotic course prescribed by a doctor. Natural support alongside that treatment improves outcomes. Natural support instead of that treatment does not.
11 Natural Remedies for Peptic Ulcer
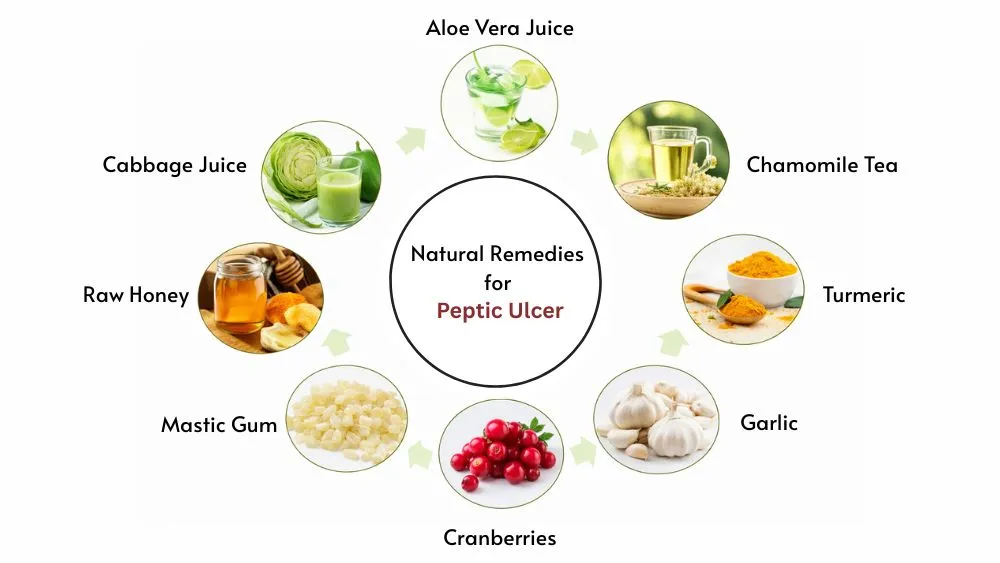
The 11 natural remedies for peptic ulcer below are sorted by the strength of evidence behind them.
1. Cabbage Juice
Cabbage contains glutamine, an amino acid that fuels the cells lining your stomach. These cells rebuild the stomach wall after ulcer damage. Fresh cabbage juice heals peptic ulcers in 10 days on average. Drink half a cup of fresh, raw cabbage juice twice daily. It does not taste good. It works.
2. Deglycyrrhizinated Licorice (DGL)
DGL is a processed form of licorice root with the compound that raises blood pressure removed. What remains stimulates mucus production in the stomach. That mucus coats the ulcer and shields it from acid. DGL chewable tablets are the standard form. Chew one or two tablets 20 minutes before meals. Do not use regular licorice candy; that form raises blood pressure with daily use.
3. Probiotics
Probiotics are live bacteria that restore balance in your gut. Specific strains, particularly Lactobacillus acidophilus and Lactobacillus reuteri, reduce H. pylori colonization in the stomach. Probiotics significantly improve H. pylori eradication rates when added to antibiotic therapy. Eat one cup of plain yogurt with live cultures daily, or take a probiotic supplement with at least 1 billion CFU.
4. Raw Honey
Raw honey, especially Manuka honey from New Zealand, has direct antibacterial effects against H. pylori. It contains hydrogen peroxide and methylglyoxal (MGO), both of which damage bacterial cell walls. A teaspoon of raw Manuka honey on an empty stomach in the morning is the commonly used approach. Regular processed honey does not have the same antibacterial potency.
5. Aloe Vera Juice
Aloe vera reduces stomach acid secretion and calms inflammation in the stomach lining. Aloe vera gel reduces gastric acid levels comparable to some standard antacids. Drink 20 ml of pure aloe vera juice, not gel, twice daily before meals. Avoid products with added sugar or aloin (a harsh laxative compound sometimes present in aloe).
6. Turmeric
Curcumin in turmeric blocks a protein called NF-kB, which drives inflammation in the stomach lining. Animal studies show curcumin reduces ulcer size. Human studies show it reduces gastric irritation. Half a teaspoon in warm water twice daily is practical. Do not exceed 1 gram of curcumin supplements per day. High doses of curcumin supplements irritate the stomach in some people, which defeats the purpose.
7. Garlic
Garlic contains allicin, a compound that inhibits H. pylori growth. Garlic extract reduces H. pylori load in the stomach significantly. Two raw garlic cloves daily, crushed and swallowed with water, is the practical dose. Cooking destroys allicin. Raw garlic on an empty stomach irritates some people; eat it with a small amount of food if needed.
8. Chamomile Tea
Chamomile reduces spasms in the digestive tract and lowers inflammation in the stomach wall. For peptic ulcer patients, it reduces the burning sensation between meals. One cup of chamomile tea between meals, not immediately after eating, works better than drinking it with food.
9. Mastic Gum
Mastic gum comes from the Pistacia lentiscus tree. It is one of the most studied natural remedies for peptic ulcer, specifically for H. pylori. A study in the New England Journal of Medicine found that 1 gram of mastic gum daily for 2 weeks killed H. pylori in test cultures. Clinical evidence in humans is moderate but promising. Mastic gum capsules are widely available in health stores.
10. Cranberries
Cranberries contain proanthocyanidins that prevent H. pylori from sticking to the stomach lining. If the bacteria cannot stick, they cannot colonize and cause damage. Unsweetened cranberry juice, 200 ml twice daily, is the effective form. Sweetened cranberry juice adds sugar, which feeds bad gut bacteria and reduces benefit.
11. Stress Reduction Techniques
Stress does not directly cause peptic ulcers but worsens them significantly. Stress increases cortisol, which reduces blood flow to the stomach lining and slows mucosal repair. Yoga, deep breathing, and 7 to 8 hours of sleep reduce cortisol and support healing. Structured meal timing, eating at the same time every day, also reduces acid spikes that irritate existing ulcers.
Diet Plan for Peptic Ulcer Recovery
A proper diet plan for peptic ulcer recovery reduces acid exposure, provides nutrients for tissue repair, and avoids further irritation.
What to Eat
- Oatmeal: Forms a gel in the stomach that coats the ulcer and reduces acid contact
- Brown rice: Easy to digest, does not spike acid
- Steamed vegetables: Broccoli, carrots, and pumpkin are low-acid and anti-inflammatory
- Lean proteins: Tofu, moong dal, and chicken breast without skin support tissue repair
- Yogurt with live cultures: Probiotics directly support stomach lining recovery
- Bananas: Stimulate mucus secretion in the stomach lining
Sample Daily Diet Plan
- Breakfast: Oatmeal with half a banana and a glass of warm water
- Mid-morning: A cup of chamomile tea or plain yogurt
- Lunch: Steamed rice, moong dal, and boiled carrots or bottle gourd
- Snack: One small banana or a small bowl of plain yogurt
- Dinner: Soft khichdi (rice and lentil porridge) or a bowl of vegetable soup with no spice
Eat every 3 to 4 hours. A stomach sitting empty for too long produces acid that hits the ulcer directly.
Foods to Avoid With Peptic Ulcer
The foods to avoid with peptic ulcer are the ones that either increase acid production or damage the stomach lining directly.
- Alcohol: Breaks down the protective mucus layer and increases acid. Even one drink slows ulcer healing measurably.
- Spicy foods: Capsaicin irritates the already raw ulcer surface and increases pain
- Fried foods: Slow digestion, keep food in the stomach longer, and increase acid production time
- Coffee: Stimulates hydrochloric acid secretion even in decaffeinated form
- Carbonated drinks: The carbon dioxide expands in the stomach, increases pressure, and pushes acid toward the ulcer
- Citrus fruits (if symptomatic): Oranges, lemon juice, and tomatoes increase acid load on an already damaged lining
- NSAIDs like ibuprofen: Directly strip the stomach’s protective lining. Switch to paracetamol for pain, with a doctor’s guidance.
Alcohol-Related Peptic Ulcer Recovery at Home
Alcohol-related peptic ulcer recovery at home starts with one non-negotiable step: stop all alcohol immediately.
Alcohol does two things to peptic ulcers. First, it dissolves the mucus layer that protects the stomach wall. Second, it increases acid secretion. Together, this exposes the ulcer to direct acid contact every time alcohol enters the stomach. Even moderate drinking, two drinks a day, increases ulcer bleeding risk by 30 to 40%.
At home, after stopping alcohol:
- Eat a high-protein diet: eggs, tofu, and moong dal to support tissue repair
- Take Vitamin B complex supplements because alcohol depletes B1, B6, and B12 significantly
- Drink enough water: 2 to 3 liters per day to support stomach lining renewal
- Monitor stool color: black or tarry stool means the ulcer is bleeding. Go to a hospital immediately.
Medical supervision is essential in alcohol-related cases. Liver function may also be compromised, which changes how well the stomach heals.
Stress-Related Stomach Ulcer Natural Treatment
Stress-related stomach ulcer natural treatment addresses the hormonal chain that worsens ulcers.
Stress raises cortisol. High cortisol reduces prostaglandin production in the stomach. Prostaglandins are the compounds that maintain the protective mucus layer. Less prostaglandin means a thinner, weaker stomach lining. Acid then reaches the ulcer surface faster and more often.
Management:
- Meditation or deep breathing for 10 minutes before meals lowers cortisol enough to reduce acid output
- Yoga poses like Vajrasana after meals improve gastric blood flow and support mucosal repair
- Adequate sleep: Less than 6 hours raises cortisol the next morning. 7 to 8 hours is the minimum.
- Avoid caffeine after 2 PM: Caffeine combined with cortisol spikes acid production more than either alone
- Eat at fixed times: Irregular meal timing creates acid spikes when the stomach expects food but gets none
How Long Does a Peptic Ulcer Take to Heal?
With proper medical treatment, most peptic ulcers heal in 4 to 8 weeks. H. pylori eradication therapy, a 14-day antibiotic course, clears the infection. Proton pump inhibitors (PPIs) like omeprazole then reduce acid while the lining repairs.
Without treatment, ulcers worsen, not improve. An untreated H. pylori ulcer can bleed, perforate (create a hole in the stomach wall), or turn into gastric cancer over the years.
Natural remedies for peptic ulcer shorten healing time when used alongside medical treatment. They do not replace it.
Warning Signs of a Complicated Ulcer
Go to a hospital immediately if you notice:
- Vomiting blood (red or coffee-ground-colored material)
- Black, tarry, or tar-smelling stool (sign of internal bleeding)
- Severe stabbing pain in the upper abdomen
- Sudden dizziness or fainting
- Rapid heart rate with sweating
These signs mean the ulcer has either bled or perforated. This is a medical emergency, not a situation for home care.
When Natural Remedies Are Not Enough
Natural remedies for peptic ulcer stop being sufficient when:
- Symptoms persist for more than 2 weeks despite dietary changes
- A breath test, stool test, or endoscopy confirms H. pylori infection
- The ulcer formed from long-term NSAID use
- You have had a bleeding ulcer before
Medical treatments include:
- Proton pump inhibitors (PPIs): Omeprazole, pantoprazole, reduce acid production significantly
- Triple therapy antibiotics: Clarithromycin, amoxicillin, and a PPI for 14 days to eradicate H. pylori
- Endoscopy: Both diagnostic and therapeutic; doctors can stop bleeding ulcers during the procedure
FAQs
Can peptic ulcers heal without medication?
Small ulcers from mild NSAID irritation sometimes heal with dietary changes and stopping the NSAID. But H. pylori ulcers do not heal without antibiotics. The bacteria stay active and reopen the ulcer. Only 5 to 10% of confirmed H. pylori ulcers show lasting recovery without antibiotic eradication.
Is milk good for ulcers?
No. Milk gives temporary relief because it neutralizes acid for 20 to 30 minutes. After that, the calcium and protein in milk trigger more acid secretion than before. This rebound acid worsens ulcer pain. Cold water or DGL licorice works better for symptom relief without the rebound.
Is turmeric safe for ulcers?
Yes, at kitchen doses. Half a teaspoon of turmeric powder in water twice daily is safe and anti-inflammatory. Curcumin supplements above 1,000 mg per day irritate the stomach lining in some people. Stick to food-level amounts of turmeric as a natural remedy for peptic ulcer, not high-dose supplements.
Can stress alone cause ulcers?
No. Stress alone does not create peptic ulcers. It worsens existing ulcers and slows healing significantly. The two confirmed causes are H. pylori infection and NSAID use. Stress is a strong aggravating factor, not an independent cause. However, ICU patients under extreme physical stress can develop “stress ulcers,” which is a separate clinical condition.
Are probiotics helpful for H. pylori?
Yes. Probiotics do not kill H. pylori alone. But Lactobacillus reuteri and Lactobacillus acidophilus reduce H. pylori colonization and improve eradication rates of antibiotic therapy by 10 to 15%. They also reduce antibiotic side effects like diarrhea, which improves treatment completion. Use them alongside antibiotics, not instead of them.














Leave a Comment