Second-degree heart block is a condition where the heart’s electrical system misfires, not completely, but enough to skip beats and disrupt rhythm. Unlike a full block, the signal between the upper and lower chambers still gets through sometimes.
The distinction between where the block occurs (the AV node versus the His-Purkinje system) changes everything about treatment and prognosis.
Second-degree heart block is a condition of two, with very different risk levels and very different outcomes. Mobitz I in an otherwise healthy person is manageable. Mobitz II in anyone requires pacemaker implantation.
If you have been diagnosed with second-degree heart block and are unclear which type you have, ask your cardiologist directly to determine your entire treatment path.
Types of Second-Degree Heart Block
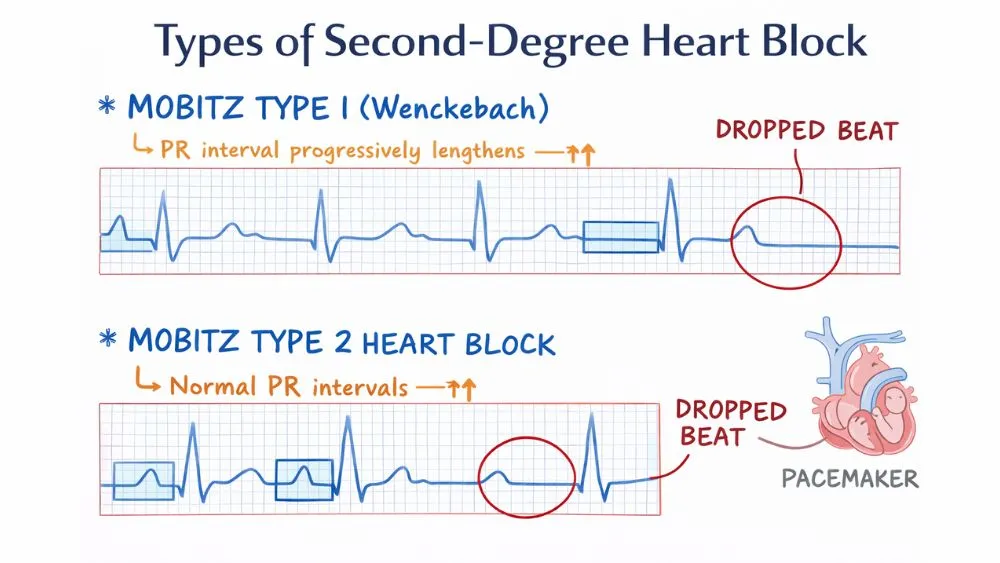
Mobitz Type I (Wenckebach)
In Mobitz Type I, the heart’s electrical signal from the upper heart chambers (atria) gets delayed a little more with each beat, until one beat fails to pass through entirely. Then the cycle resets and starts again.
This pattern is called Wenckebach. It is often found in trained athletes, younger people, and during sleep when the heart rate naturally slows. In isolation, without symptoms, it rarely requires treatment.
Mobitz Type 2 Heart Block
Mobitz type 2 heart block does not follow a pattern. The PR interval on the ECG stays the same, then a beat just drops without a warning symptom.
Mobitz type 2 heart block can progress to complete (third-degree) heart block without any notice. When that happens, the heart’s lower chambers stop receiving signals altogether and can stop pumping effectively.
Mobitz type 2 heart block accounts for fewer overall cases of second-degree block, but it carries a significantly higher risk of sudden cardiac arrest. Most cardiologists treat it as a pacemaker indication regardless of symptoms.
Second-Degree Heart Block Symptoms
Second-degree heart block symptoms depend on how often the heartbeats drop and how the body compensates.
Common second-degree heart block symptoms include:
- Dizziness: The brain gets a fraction less blood during a dropped beat; repeat this dozens of times daily, and dizziness becomes constant
- Lightheadedness: Especially when standing up quickly
- Fatigue: The heart pumps less efficiently overall, so the body tires faster
- Shortness of breath: Especially with mild exertion
- Syncope (fainting): A dropped beat at the wrong moment drops blood pressure enough to lose consciousness
- Palpitations: A fluttering or skipping sensation in the chest
You may have Mobitz I with zero second-degree heart block symptoms. It gets picked up during a routine ECG or a check-up for something else entirely. This is common in athletes.
Mobitz II is more likely to cause symptoms. If syncope or near-fainting episodes are happening, that is a medical emergency.
Second-Degree Heart Block Causes
Second-degree heart block causes fall into four main categories. Identifying the cause determines whether the block is reversible or permanent.
Ischemic Heart Disease
A heart attack damages the heart muscle and conduction tissue together. The inferior wall of the heart (supplied by the right coronary artery) is the most common site. Inferior myocardial infarction frequently produces Mobitz I. Anterior MI produces Mobitz II, which carries worse outcomes.
Degenerative Conduction Disease
Aging causes fibrosis (scarring) in the heart’s conduction pathways. This is Lev’s disease, or Lenègre disease, the slow, progressive replacement of electrical tissue with non-conducting scar tissue. It is the most common second-degree heart block cause in adults over 60 with no other cardiac disease.
Medication-Induced
Three drug classes slow conduction through the AV node:
- Beta-blockers (metoprolol, atenolol): Reduce heart rate and slow AV conduction
- Calcium channel blockers (diltiazem, verapamil): Directly suppress AV node activity
- Digoxin: Increases vagal tone; at toxic levels, causes almost any arrhythmia
Drug-induced heart block is often reversible. Stopping or reducing the offending medication resolves the block in many cases within 24–72 hours.
Electrolyte Imbalance
Hyperkalemia (too much potassium in the blood) disrupts the electrical charge of cardiac cells. Potassium above 6.5 mEq/L can produce PR prolongation, widened QRS complexes, and AV block. This is a medical emergency. It occurs in kidney failure, Addison’s disease, and in patients over-supplementing potassium.
Second-Degree Heart Block ECG
Reading a second-degree heart block ECG is about pattern recognition.
Mobitz I ECG Pattern
- The PR interval (the gap between the P wave and QRS complex) gets longer with each beat
- After several beats, a QRS drops entirely, indicating no ventricular contraction
- The next cycle starts with a shorter PR interval and repeats
The second-degree heart block ECG in Mobitz I has progressively wider PR gaps until one QRS disappears. If you count the beats, the ratio is often 3:2 or 4:3 (3 P waves to 2 QRS complexes, for example).
Mobitz II ECG Pattern
- The PR interval stays exactly the same from beat to beat
- Without any warning, a QRS drops suddenly
This second-degree heart block ECG pattern is more ominous precisely because it is unpredictable. The block occurs below the AV node (in the bundle of His or bundle branches), which makes progression to complete block more likely.
2:1 AV Block
Every other P wave gets blocked. Two P waves per one QRS. This pattern is tricky because you cannot tell from the ECG alone whether it is Mobitz I or Mobitz II. Clinical context and additional testing determine which type underlies the 2:1 block.
Second-Degree Heart Block Treatment
Second-degree heart block treatment depends entirely on the type, the cause, and whether the patient has symptoms.
Mobitz I Management
Most cases of Mobitz I require no treatment beyond monitoring. If a reversible cause exists (a medication, an electrolyte problem, a recent inferior MI), correcting that cause often resolves the block. Asymptomatic Mobitz I in a young athlete with a slow resting heart rate is almost never treated.
Mobitz II Management
Second-degree heart block treatment for Mobitz II requires permanent pacemaker implantation. It is the standard recommendation for most patients, even without symptoms, because the risk of sudden progression to complete block is too high to manage conservatively. The 2013 ACC/AHA guidelines on pacemaker implantation classify symptomatic Mobitz II as a Class I indication (highest recommendation level).
Acute Symptomatic Cases
If a patient arrives at the ER with a symptomatic block (fainting, low blood pressure, very slow heart rate):
- Atropine 0.5–1 mg IV is given first. It blocks vagal tone and can speed up AV conduction temporarily. It works better for Mobitz I than Mobitz II.
- Transcutaneous pacing: Electrical pacing delivered through chest pads is used when atropine fails or the block is severe. It bridges the patient until a permanent pacemaker is placed.
When Is Second Degree Heart Block Dangerous?
Three situations push second-degree heart block into emergency territory:
- Syncope: Fainting from a dropped beat means the block is causing real hemodynamic impact
- Hemodynamic instability: Blood pressure drops, heart rate too slow to sustain circulation
- Progression to complete heart block: Third-degree block means no signals get through at all; the ventricles pace themselves slowly and inefficiently; without a pacemaker, cardiac output collapses
Mobitz II in any patient with a history of anterior MI is treated as a pending emergency, even if the patient feels fine.
Diagnosis and Monitoring
- 12-lead ECG: The first and most important tool identifies the pattern and type
- Holter monitor: A 24–48 hour continuous ECG worn at home; catches intermittent blocks that a clinic ECG might miss
- Echocardiogram: Ordered when structural heart disease is suspected; checks heart function, wall motion, and valves
A single ECG can miss intermittent Mobitz II. If symptoms are present but the ECG is clean, a Holter monitor is the next step.
FAQs on Second Degree Heart Block
Is second-degree heart block serious?
Mobitz I is usually benign and often needs no treatment. Mobitz II carries a real risk of sudden progression to complete heart block, which can cause cardiac arrest without warning. Never assume they are in the same condition.
Which is more dangerous, Mobitz I or II?
Mobitz II is significantly more dangerous. It blocks below the AV node in the His-Purkinje system, making a complete block more likely. Mobitz I blocks at the AV node itself and rarely progresses. Most cardiologists implant a pacemaker for Mobitz II regardless of symptoms.
Can a second-degree heart block go away?
Yes, if the cause is reversible. Drug-induced block from beta-blockers or digoxin often resolves within 24–72 hours of stopping the medication. Hyperkalemia-related block resolves when potassium normalizes. Post-MI Mobitz I after an inferior heart attack often resolves within 1–2 weeks.
Does Mobitz II require a pacemaker?
Yes. The ACC/AHA guidelines classify symptomatic second-degree heart block Mobitz II, as a Class I pacemaker indication. Even asymptomatic patients often receive a pacemaker because the risk of sudden complete block outweighs the risk of the procedure.
Can it cause fainting?
Yes. A dropped beat lowers cardiac output briefly. When beats drop frequently enough (especially during exertion), blood pressure falls, and fainting follows. Syncope from second-degree heart block is a red flag requiring same-day evaluation, not a scheduled appointment.
What does 2:1 AV block mean?
Every second P wave gets blocked; for every two atrial beats, and only one ventricular beat follows. The ECG alone cannot confirm whether it is Mobitz I or II in this pattern. A longer rhythm strip, increased heart rate with exercise, or vagal maneuvers help differentiate the two types clinically.
Can athletes have Mobitz I?
Yes. Highly trained endurance athletes (marathon runners, cyclists) have elevated vagal tone that slows AV conduction. Mobitz I found during sleep or rest in a fit, asymptomatic athlete with no structural heart disease is considered a normal variant and does not require treatment.
Is second-degree heart block reversible?
Partially. Drug-induced and electrolyte-related blocks are reversible. Degenerative fibrosis from aging is not. Post-MI blocks sometimes resolve, sometimes become permanent. The underlying cause determines reversibility, not the block type alone.
How is it diagnosed?
A standard 12-lead ECG catches most cases. Intermittent second-degree heart block requires a Holter monitor for 24–48 hours. If structural disease is suspected, an echocardiogram follows. Electrolyte panels and a medication review are standard in all new diagnoses.
When should I go to the ER?
Go to the ER immediately if you faint, nearly faint, feel your heart beat very slowly and irregularly, or have chest pain with breathlessness. Second-degree heart block causing syncope is treated as a potential complete block until proven otherwise. Do not drive yourself.











Leave a Comment