Depression can cause headaches, and the connection is neurological. Major depressive disorder alters brain chemistry in ways that directly trigger head pain.
A 2021 study published in The Journal of Headache and Pain found that people with depression are three times more likely to develop chronic headaches than those without it. The relationship runs both ways; headaches worsen depression, and depression worsens headaches.
Can Mental Health Cause Physical Headaches?
Mental health can cause physical headaches. The brain doesn’t separate emotional pain from physical pain. Both use the same neural pathways. When depression disrupts those pathways, physical symptoms like headaches, body aches, and fatigue follow. This is called somatization, and it’s one of the most documented but least explained aspects of depression in mainstream health content.
Brain-Body Connection Explained
The brain’s limbic system controls both emotion and pain perception. Depression changes how the limbic system processes signals. When the limbic system is dysregulated by depression, it sends pain signals through the trigeminal nerve, which is the same nerve responsible for most headaches. This is why depression-related headaches aren’t just “stress headaches.” They have a direct neurological origin.
How Emotional Stress Becomes Physical Pain
Chronic emotional stress activates the body’s HPA (hypothalamic-pituitary-adrenal) axis. This raises cortisol levels. Elevated cortisol tightens muscles around the skull and neck, inflames blood vessels, and lowers the brain’s pain threshold. The result is physical head pain, driven entirely by an emotional and hormonal process.
Why Mental Health Symptoms Show Up as Headaches
Serotonin regulates both mood and pain sensitivity. Depression depletes serotonin. Low serotonin makes the brain hypersensitive to pain signals. So a level of muscle tension that would be unnoticeable in a healthy brain registers as a full headache in someone with depression. This explains why depression-related headaches feel disproportionate to any physical cause.
How Depression Triggers Headaches
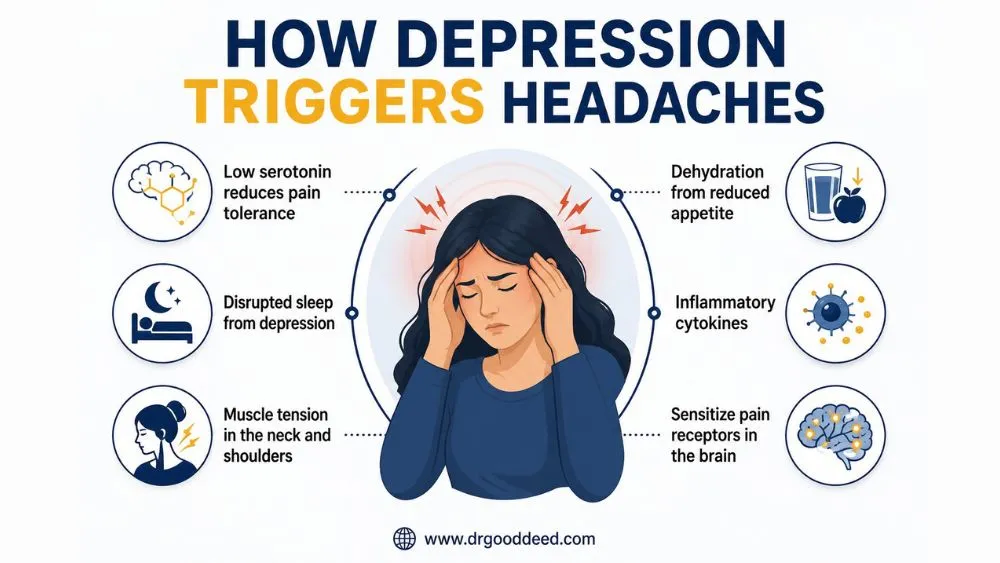
Depression can cause headaches through specific biological triggers. The mechanism involves three overlapping systems working against each other.
Stress hormones causing headaches is one of the most direct paths. Cortisol and adrenaline, released during depressive episodes, constrict blood vessels in the brain. When those vessels dilate afterward, the expansion causes throbbing pain. This is identical to the mechanism behind vascular migraines.
Key depression-to-headache triggers:
- Low serotonin reduces pain tolerance across the entire body
- Disrupted sleep from depression causes next-day tension headaches
- Muscle tension in the neck and shoulders, common in depression, compresses nerves
- Dehydration from reduced appetite and low motivation worsens head pain
- Inflammatory cytokines, elevated in depression, sensitize pain receptors in the brain
Depression Related Headache Types
Depression related headache types fall into three main categories. Most online sources don’t distinguish between them. Knowing which type is happening changes how it gets treated.
Tension Headaches (Most Common)
Tension headaches are the most frequent depression related headache type. They feel like a tight band around the head. The pain is dull and constant, usually bilateral, meaning it affects both sides. Muscle tension from depression in the neck, scalp, and jaw directly causes these. They can last 30 minutes to several hours. People with untreated depression report tension headaches almost daily.
Migraine Linked to Depression
Depression and migraine share overlapping brain chemistry. Both involve serotonin dysregulation. Research from Harvard Medical School found that people with major depression are 40% more likely to develop migraines. These headaches are typically one-sided, throbbing, and accompanied by nausea or light sensitivity. The link is bidirectional; migraine sufferers are also more likely to develop depression.
Chronic Daily Headaches
Chronic daily headaches are defined as headaches occurring 15 or more days per month. Depression is one of the leading psychiatric causes. These often develop when tension headaches go untreated and become a permanent cycle. Overusing pain medication to manage them creates rebound headaches, making the problem significantly worse.
Symptoms That Suggest Depression-Related Headaches
These symptoms together, rather than individually, indicate the headache source is depression rather than a physical condition.
Persistent Dull or Pressure-Like Pain
The pain isn’t sharp or stabbing. It’s a heavy, dull pressure. People often describe it as wearing a tight hat that won’t come off. This pattern is characteristic of tension-type headaches driven by muscle contraction from chronic low mood.
Headaches With Fatigue and Low Mood
A headache that consistently arrives alongside exhaustion and emotional flatness points to depression as the source. Physical headaches from dehydration or illness clear up. Depression headaches tend to persist or return the following day.
Pain Worsens With Stress or Emotional Triggers
If a difficult conversation, stressful news, or emotional conflict makes the headache worse within minutes, stress hormones causing headaches is the active mechanism. This pattern rarely occurs with structural or neurological headaches.
Sleep Problems Alongside Headaches
Depression disrupts slow-wave sleep. Missing deep sleep prevents the brain from clearing metabolic waste and recovering pain thresholds. Waking up with a headache after a full night of poor-quality sleep is a reliable signal that depression is involved.
How to Treat Depression Related Headaches
Treating depression-related headaches requires treating the depression itself. Targeting only the headache with pain medication provides short-term relief and creates long-term dependency. The headache is a symptom. The depression is the root.
Treating the Root Cause: Depression Management
Medications for depression and headaches overlap more than most people realize. SSRIs like fluoxetine and sertraline raise serotonin, which reduces both depressive symptoms and pain sensitivity. SNRIs like venlafaxine are specifically used for both depression and chronic headache prevention. Tricyclic antidepressants cause low, particularly amitriptyline, are first-line treatments for chronic tension headaches and depression combined.
Therapy: CBT and Stress Management
Cognitive Behavioral Therapy (CBT) reduces the frequency of tension headaches in people with depression by addressing the thought patterns that sustain muscle tension and cortisol elevation. A 2019 meta-analysis in Cephalalgia found CBT reduced headache days by an average of 30% in patients with comorbid depression.
Sleep and Lifestyle Correction
Fixing sleep is non-negotiable. Poor sleep sustains both depression and headaches. Consistent sleep timing, limiting screens after 9 PM, and avoiding alcohol improve sleep architecture within 2 weeks. Regular aerobic exercise for 30 minutes daily raises endorphins and reduces cortisol, addressing both conditions simultaneously.
Physical Relaxation Techniques
Progressive muscle relaxation targets the neck and scalp tension that causes tension headaches directly. Biofeedback therapy, which teaches patients to control muscle tension consciously, reduced headache frequency by 45% in clinical trials at the Cleveland Clinic. These approaches work because they address the muscular component of depression headaches that medication alone doesn’t reach.
What Makes Depression Headaches Worse
Specific behaviors reliably worsen depression related headache types and are mostly avoidable.
Depression can cause headaches to become chronic when these factors are present:
- Overusing ibuprofen or acetaminophen more than 10 days per month creates medication overuse headache on top of depression headaches
- Skipping meals drops blood sugar, which triggers vasodilation and head pain
- Caffeine withdrawal after regular use causes rebound headaches
- Social isolation worsens both depression severity and headache frequency
- Untreated sleep apnea, common in depression, causes morning headaches from oxygen disruption overnight
- Screen time before bed delays melatonin release, reducing sleep quality and raising next-day headache risk
When to See a Doctor
Depression can cause headaches severe enough to need immediate attention in specific situations.
See a doctor promptly if:
- Headaches occur more than 15 days per month
- The pain is sudden and severe, described as “the worst headache of my life”
- Headaches come with vision changes, confusion, or weakness on one side
- Current antidepressants aren’t reducing headache frequency after 6 weeks
- You’re using OTC pain medication more than 3 times per week
Routine evaluation is appropriate when depression and headaches occur together consistently. A neurologist and psychiatrist working together produce better outcomes than treating each condition separately.
FAQs
Can depression cause headaches every day?
Yes. Depression can cause headaches daily. Untreated depression with chronic cortisol elevation and low serotonin produces headaches 15 or more days per month in 30% of patients, according to research published in Neurology. These are classified as chronic daily headaches and require treating the depression, not just the pain.
Can mental health cause physical headaches?
Yes. Mental health can cause physical headaches through serotonin depletion, cortisol elevation, and trigeminal nerve sensitization. These aren’t psychosomatic headaches in the dismissive sense. They have a measurable neurochemical cause. Brain scans of depressed patients show altered pain processing in the same regions that generate headaches.
What types of headaches are linked to depression?
Depression related headache types include tension-type headaches (bilateral, pressure-like, most common), migraines (unilateral, throbbing, with nausea), and chronic daily headaches (15-plus days per month). Each type has a different treatment approach, which is why diagnosis matters before starting treatment.
How do stress hormones cause headaches?
Stress hormones causing headaches works through two pathways: cortisol tightens pericranial muscles, and adrenaline constricts then dilates cerebral blood vessels. That dilation phase produces throbbing pain. In depression, cortisol stays elevated longer because estrogen’s regulatory effect on cortisol is weakened.
How to treat depression related headaches effectively?
Treating depression-related headaches most effectively combines an SNRI like venlafaxine with CBT and aerobic exercise. Venlafaxine is FDA-recognized for both depression and headache prevention. CBT reduces headache days by 30%. Exercise raises endorphins within 20 minutes of starting. All three together outperform any single approach.
Do antidepressants help with headaches?
Yes. Medications for depression and headaches overlap significantly. Amitriptyline reduces chronic tension headache frequency by 50% and treats depression. Venlafaxine prevents migraines while treating depression. SSRIs alone are less effective for headache prevention but help when depression is the primary driver of pain sensitivity.
Why do headaches worsen with depression?
Depression lowers serotonin, which raises pain sensitivity across the entire nervous system. A muscle tension level that’s normally tolerable becomes painful when serotonin is low. Depression can cause headaches to become more intense over time, and the longer depression goes untreated, the lower serotonin falls, and the worse headaches become.
Can migraines be caused by depression?
Yes. Depression and migraine share serotonin dysregulation as a common mechanism. Harvard research found depressed patients face a 40% higher migraine risk. Depression can cause headaches classified as migraines, particularly in women, where estrogen fluctuations further deplete serotonin and increase migraine vulnerability during depressive episodes.
When should you see a doctor for depression headaches?
See a doctor when headaches exceed 15 days per month, when OTC medication use exceeds 10 days per month, or when headaches don’t improve after 6 weeks of treating depression. Mental health can cause physical headaches severe enough for emergency care when sudden severe onset occurs with neurological symptoms.
Are depression headaches different from normal headaches?
Yes. Depression-related headache types are persistent, recur with emotional triggers, improve when mood improves, and don’t fully respond to standard pain medication. Normal tension headaches clear with hydration, rest, or ibuprofen. Depression headaches return within 24 hours. That pattern of recurrence is the clearest distinguishing feature.













