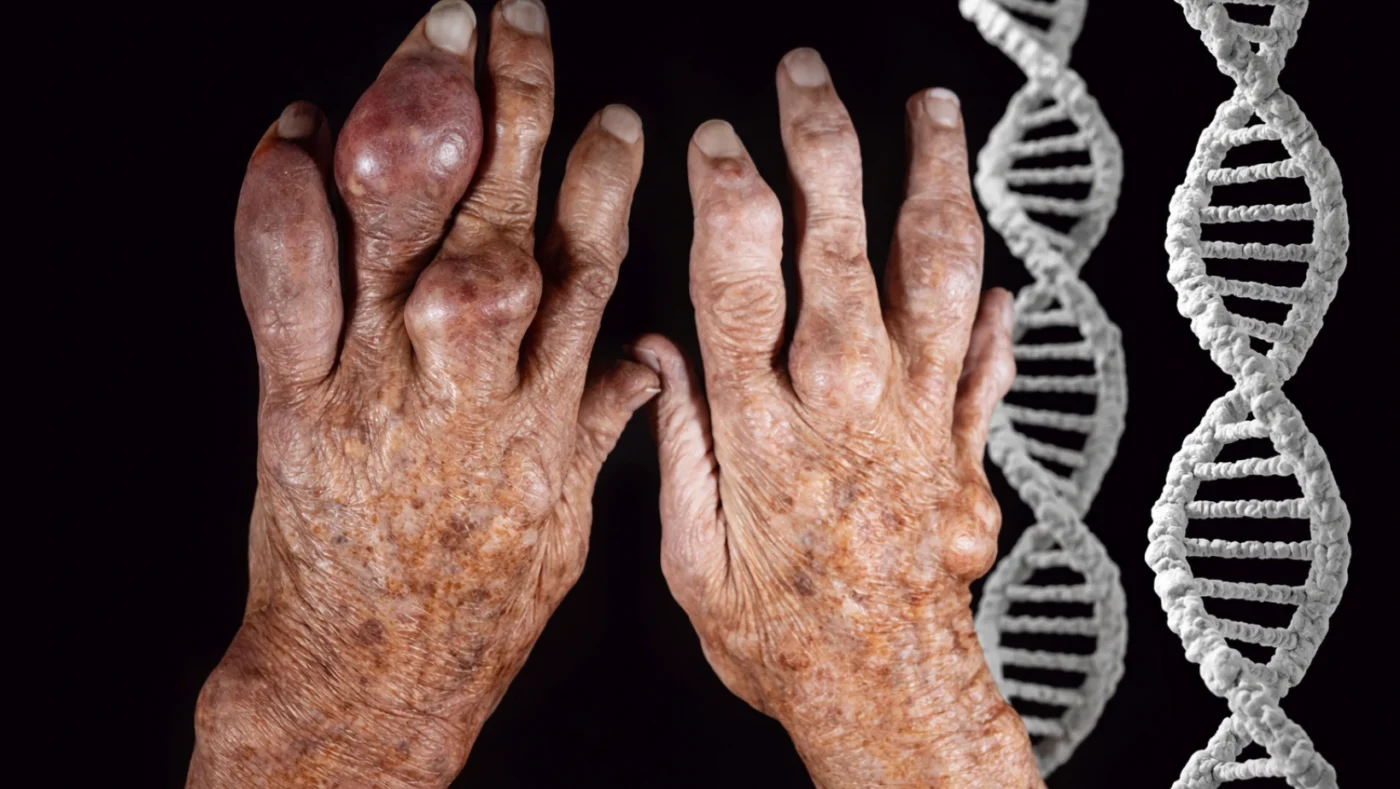
Gout is partly hereditary. Genetic variants that affect how the body handles uric acid increase gout risk significantly, but genes alone don’t cause gout. Having a parent with gout raises your risk by 20%, and carrying specific gene mutations (ABCG2, SLC2A9) raises it further.
If gout is partly hereditary in your family, the genes create the predisposition; the daily choices determine the outcome. Most people with a genetic gout risk who address uric acid early, through monitoring, diet adjustment, and medication when needed, never develop the joint damage that older generations faced.
Is Gout Hereditary?
Gout is partly hereditary, not entirely. Gout is a complex disease. Genes set the baseline risk, but lifestyle factors determine whether gout actually appears. Research shows that genetic factors account for roughly 40 to 73% of serum uric acid variation. So genetics load the gun; diet, alcohol, and weight pull the trigger.
A person with two gout-risk gene variants and a clean diet may never develop gout. A person with just one variant and daily beer consumption almost certainly will. The interaction matters more than either factor alone.
How Genetics Influence Gout Risk
Genetic causes of gout work through uric acid regulation. The body produces uric acid as it breaks down purines. Kidneys then filter and excrete it. When genes controlling either process are defective, uric acid accumulates.
Role of Uric Acid Metabolism Genes
Certain gene variants either increase uric acid production or reduce kidney excretion. Both outcomes raise serum uric acid above the crystallization threshold of 6.8 mg/dL.
Kidney Function and Urate Excretion
The kidneys handle about 70% of uric acid excretion. Gene mutations in urate transporter proteins reduce how efficiently kidneys clear uric acid. Even with a normal diet, a person with poor transporter gene function will trend toward higher-than-average uric acid levels.
Family History and Inherited Risk Patterns
Gout doesn’t follow a simple dominant or recessive inheritance pattern. Multiple genes contribute, each adding small increments of risk. A 2018 study published in Nature Genetics identified 183 genetic loci associated with serum uric acid levels. Having a first-degree relative with gout roughly doubles the baseline risk.
Why doesn’t everyone with the genes develop gout
Gene variants create predisposition, not certainty. A person carrying ABCG2 risk variants but drinking no alcohol, eating low-purine foods, and maintaining a healthy body weight often has uric acid levels that stay well below the crystallization threshold.
Key Genes Linked to Gout
SLC2A9 Gene (Urate Transport)
SLC2A9 encodes a protein that controls how much uric acid the kidneys reabsorb back into the blood after filtering. Variants in this gene cause excessive reabsorption. Less uric acid leaves the body; more stays in the blood. SLC2A9 variants are the strongest single genetic cause of gout identified so far, accounting for 3 to 4% of uric acid variation in genome-wide studies.
ABCG2 Gene (Urate Excretion Issues)
ABCG2 controls uric acid secretion from intestinal cells into the gut for excretion. When ABCG2 is dysfunctional, uric acid that should leave through the gut gets retained. The Q141K variant of ABCG2 is especially common in East Asian and South Asian populations, which explains the higher gout prevalence in those groups compared to European populations at similar dietary exposure levels.
SLC22A12 and Other Transporter Genes
SLC22A12 (URAT1) is the primary urate reabsorption transporter in kidney tubules. Loss-of-function mutations in SLC22A12 actually protect against gout by reducing reabsorption. Gain-of-function variants do the opposite. Other transporters, including SLC17A1 and SLC16A9, also modulate urate levels through overlapping pathways.
How These Genes Increase Uric Acid Levels
All four major gout genes converge on one outcome: less uric acid leaves the body than enters. Each defective transporter gene shifts the balance by 0.2 to 1.5 mg/dL on average. In a person carrying two or three of these variants, serum uric acid can sit chronically at 8 to 9 mg/dL without any dietary excess at all.
Purine Metabolism Disorders and Hereditary Gout
Purine metabolism disorders hereditary gout is a category most articles skip, but it’s clinically important.
How Purine Breakdown Affects Uric Acid
Every cell in the body contains DNA. When cells die, their DNA breaks down into purines, which then convert to uric acid. This internal production accounts for about two-thirds of the body’s uric acid. The remaining third comes from diet.
Rare Inherited Metabolic Disorders
Lesch-Nyhan syndrome is caused by a complete deficiency of HPRT1 enzyme (hypoxanthine-guanine phosphoribosyltransferase). This causes extreme uric acid overproduction and severe gout by age 10. Partial HPRT1 deficiency causes Kelley-Seegmiller syndrome, presenting as early-onset gout without the neurological features. These conditions are rare but confirm that purine metabolism disorders, such as hereditary gout, exist as a distinct clinical category.
Overproduction vs Under-Excretion of Uric Acid
About 90% of gout cases involve under-excretion by the kidneys. Only 10% involve actual overproduction. Genetic testing can identify which mechanism applies, since the treatment approach differs. Allopurinol targets overproduction; probenecid targets under-excretion.
Early Onset Gout With Family History
Early-onset gout with family history before age 30 in men or before menopause in women is a red flag for a strong genetic component.
Signs of Gout Appearing at a Younger Age
Most gout appears in men between age 40 and 60. When a man develops gout at 22, or a woman at 35, genetic predisposition is almost certainly driving it. Early-onset gout with family history needs genetic evaluation, not just dietary counseling.
Strong Genetic Predisposition Indicators
- First gout attack before age 30
- Multiple affected relatives across generations
- Gout with no clear dietary trigger
- Tophi appearing within the first few years of diagnosis
- Serum uric acid above 10 mg/dL despite normal diet
When Early Gout Suggests Hereditary Risk
If a 25-year-old develops gout with no alcohol use and a low-purine diet, testing for ABCG2 and URAT1 mutations gives diagnostic clarity and guides long-term treatment choices.
Severe Gout Symptoms and Genetic Risk
Severe gout symptoms and hereditary risk produce a more aggressive clinical course than diet-only gout.
Why Some People Develop Severe Gout
Carrying two or more high-risk gene variants keeps baseline uric acid higher between flares. The crystal burden accumulates faster. Patients with severe gout symptoms who have a hereditary risk tend to develop tophi within 5 years rather than the typical 10 to 20 years in diet-driven cases.
Frequent Flare-Ups and Chronic Gout
Genetic gout patients average 4 to 6 flares per year when untreated, compared to 1 to 2 flares in diet-only gout patients. Frequency correlates directly with baseline serum uric acid; higher baseline means more crystal deposition between attacks.
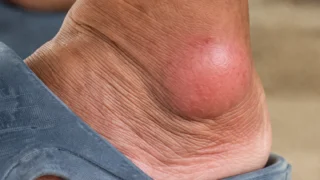
Tophi Formation and Joint Damage
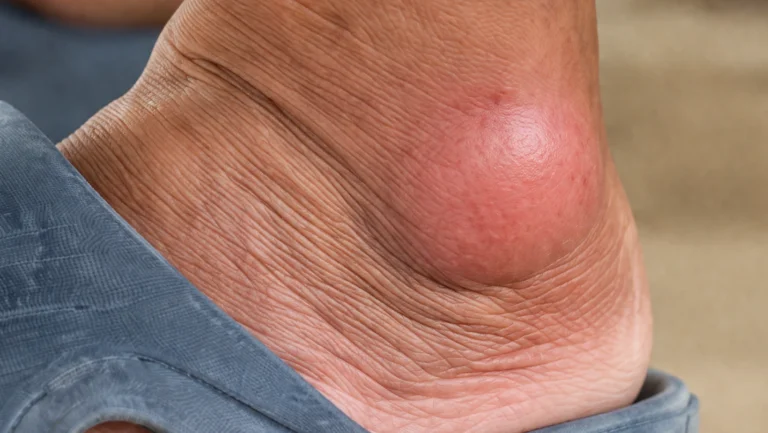
Tophi (chalky crystal deposits under the skin) form when uric acid stays above 8 mg/dL for extended periods. Genetic patients hit this threshold earlier and maintain it longer, making tophi more likely. Tophi over joints cause bone erosion with a specific radiographic pattern: punched-out lesions with overhanging edges.
Role of Genetics in Disease Progression
ABCG2 Q141K variant carriers progress to chronic tophaceous gout about 3 times faster than non-carriers at the same dietary purine intake. This is why two people eating the same foods have completely different gout trajectories.
Lifestyle vs Genetics: What Matters More
Gout is partly hereditary and lifestyle-driven.
Diet and Alcohol vs Inherited Risk
A person carrying ABCG2 risk variants who stops alcohol completely and eliminates organ meats often brings uric acid from 8.5 mg/dL down to 6.2 mg/dL through diet alone. Genetics set the ceiling; lifestyle determines whether that ceiling gets hit.
Obesity and Metabolic Syndrome Impact
Adipose (fat) tissue produces uric acid as a byproduct of fat cell metabolism. BMI above 30 raises uric acid independently of diet. Insulin resistance (common in metabolic syndrome) reduces kidney urate excretion by a measurable 15 to 25%.
Environmental Triggers Overriding Genetics
Surgery, severe illness, or starting a diuretic medication can trigger gout even in low-genetic-risk individuals. In high-genetic-risk individuals, these triggers cause faster and more severe flares.
Why Lifestyle Control Is Still Critical
Genetic risk doesn’t make gout inevitable or unmanageable. It means the margin for error is smaller. A low-genetic-risk person can drink beer weekly without issue; a high-genetic-risk person likely cannot.
Managing Hereditary Gout Risk
Managing hereditary gout risk requires both medication and lifestyle adjustments, since lifestyle alone often won’t fully correct genetically elevated uric acid.
For patients with confirmed genetic gout risk:
- Start uric acid monitoring annually after age 25 if there’s a family history
- Target serum uric acid below 6 mg/dL; below 5 mg/dL if tophi are present
- Allopurinol (first-line): starts at 100 mg/day, titrated up to 300 to 600 mg/day based on uric acid response
- Febuxostat: used when allopurinol causes side effects; more effective in ABCG2 variant carriers
- Drink 2.5 to 3 liters of water daily; this alone lowers uric acid by 0.3 to 0.5 mg/dL
- Avoid beer completely; it combines two uric acid-raising mechanisms in one drink
- Tart cherry extract (1000 mg daily) reduces flare frequency by approximately 35% based on clinical studies
Can Genetic Testing Predict Gout?
When Testing Is Useful
Genetic testing adds real value in three situations: early-onset gout before age 30, severe or rapidly progressing gout with tophi appearing within 5 years, and gout in a person with no clear dietary or lifestyle triggers.
Limitations of Genetic Screening
Current genetic tests identify variants that explain roughly 7 to 10% of uric acid heritability. The remaining genetic contribution comes from hundreds of smaller-effect variants not yet captured in standard panels. A negative test doesn’t rule out hereditary risk.
Clinical Relevance in Real Practice
Most Indian rheumatologists use genetic testing selectively rather than routinely. It changes treatment choice mainly in early-onset cases or when standard medications fail. Standard serum uric acid monitoring remains more practical for the majority of patients.
Who Is Most at Risk
Family History of Gout
A parent with gout raises risk by 20%. Two parents with gout raises it by 40%. First-degree relatives of patients with severe gout symptoms hereditary risk should start uric acid monitoring by age 25.
Men vs Women Differences
Men develop gout at 4 times the rate of premenopausal women. Estrogen promotes uric acid excretion. After menopause, women’s uric acid rises and matches male levels, increasing gout risk sharply.
Ethnic and Genetic Susceptibility
Maori populations in New Zealand carry ABCG2 risk variants at high frequency and have gout prevalence of 6 to 10%, far above global averages. South Asian and East Asian populations also carry higher rates of ABCG2 Q141K mutations than European populations.
Co-Existing Conditions
Hypertension, chronic kidney disease, Type 2 diabetes, and hypothyroidism all raise gout risk independently. When these conditions stack onto genetic predisposition, gout becomes very likely without proactive management.
When to See a Doctor
If gout is partly hereditary in your family, get a serum uric acid test immediately if a first-degree relative has been diagnosed with gout. Don’t wait for a flare.
See a doctor right away if:
- A joint becomes hot, red, and painful overnight with no injury
- You have a family history of gout and uric acid tests come back above 7 mg/dL
- A first gout attack happens before age 35
- Flares occur more than twice in 12 months
- Small white or chalky lumps appear near joints (tophi)
- You take diuretics (thiazides, furosemide) and have a gout family history; these medications raise uric acid and accelerate genetic risk significantly
A rheumatologist handles complex hereditary cases. A general physician manages straightforward first-time flares.
Frequently Asked Questions
If my parents have gout, will I get it?
Gout is partly hereditary from one parent. Having one parent with gout raises your risk by about 20%. But without dietary triggers like beer, organ meats, or obesity, many people with a positive family history never develop a single flare.
Can gout skip generations?
Yes. Gout-risk genes follow a polygenic (multi-gene) inheritance pattern, not a simple dominant one. A child can inherit fewer risk variants than a parent and remain symptom-free their entire life, while a grandchild inherits the full combination and develops gout early.
Is hereditary gout more severe?
Yes. Patients with ABCG2 Q141K mutations develop tophi roughly 3 times faster than diet-driven gout patients. Severe gout symptoms also produces higher baseline uric acid levels, typically 8 to 10 mg/dL, which means more crystal accumulation between flares.
Can lifestyle prevent genetic gout?
Yes, in many cases. Eliminating beer, reducing organ meat intake, maintaining BMI below 25, and drinking 3 liters of water daily lowers uric acid by 1 to 2 mg/dL. For patients with borderline genetics, this is often enough to stay below the 6.8 mg/dL crystallization threshold.
What age does hereditary gout start?
Diet-driven gout typically starts between age 40 and 60. Hereditary gout with strong gene variants, especially complete HPRT1 deficiency in Lesch-Nyhan syndrome, can appear in childhood. ABCG2-linked early-onset gout with family history typically presents in the late 20s to mid-30s.
Can children develop gout due to genetics?
Yes. Lesch-Nyhan syndrome causes gout by age 10. Partial HPRT1 deficiency (Kelley-Seegmiller syndrome) causes gout before age 20 in some patients. These are rare but real presentations of purine metabolism disorders hereditary gout.
How do I reduce my genetic risk of gout?
Get a serum uric acid test annually starting at age 25. Keep uric acid below 6 mg/dL. Avoid beer (highest risk trigger), organ meats, and sardines. Eat low-fat dairy daily; casein in dairy actively lowers uric acid. If uric acid stays above 7 mg/dL despite diet changes, start allopurinol.
Is genetic gout curable?
No, but it is fully manageable. The genetic variant remains, but you can keep uric acid levels low enough to prevent crystals from forming by using allopurinol or febuxostat Patients on consistent urate-lowering therapy have zero flares for years.
Should I get tested if gout runs in my family?
Yes. A basic serum uric acid blood test costs under 300 rupees in most Indian diagnostic labs. Get it done at age 25 if a parent has gout. If it comes back above 6.5 mg/dL, act on diet immediately. Genetic panel testing is useful only if uric acid is high with no dietary explanation.
What foods should I avoid if I have genetic risk?
Avoid beer (fastest uric acid trigger), organ meats (liver, kidneys), sardines, anchovies, mussels, and any drinks containing high-fructose corn syrup. These foods raise uric acid the fastest in people with genetic predisposition. Low-fat dairy, eggs, vegetables, and coffee are safe and actively lower uric acid.







Leave a Comment