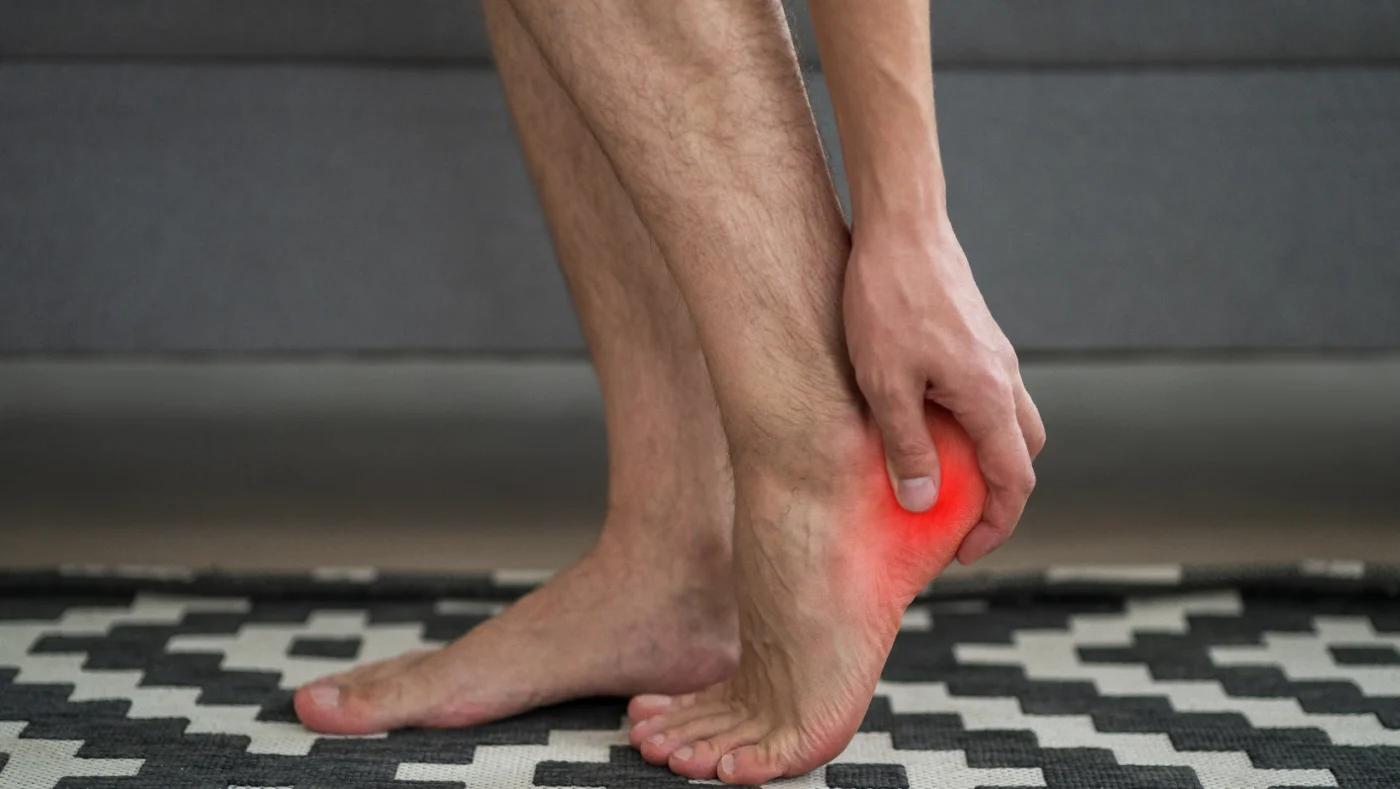
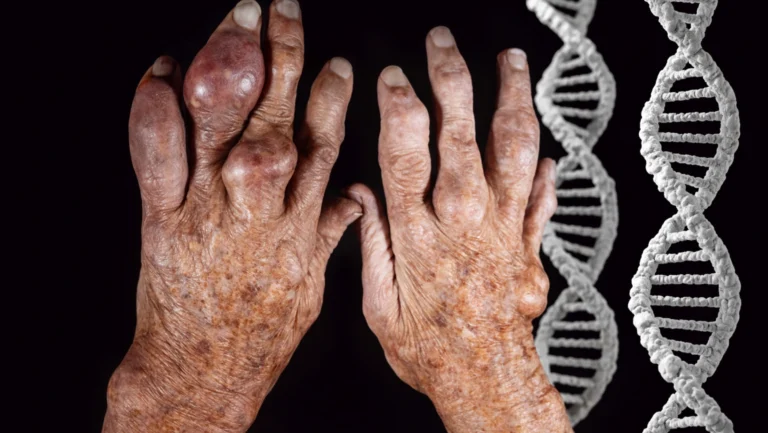
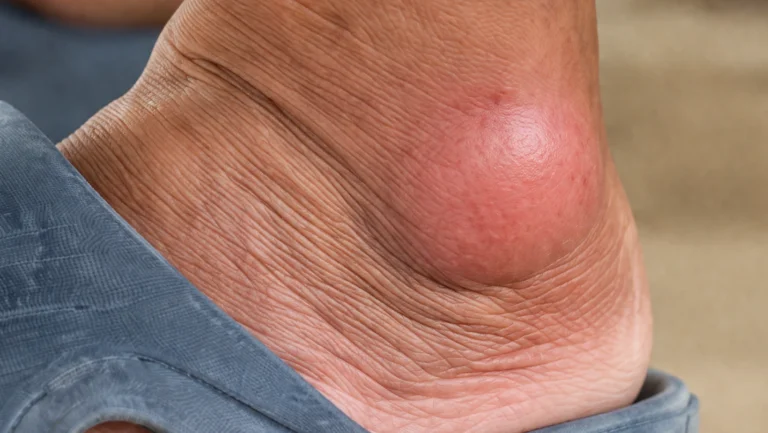
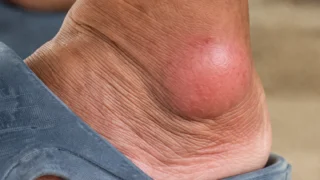
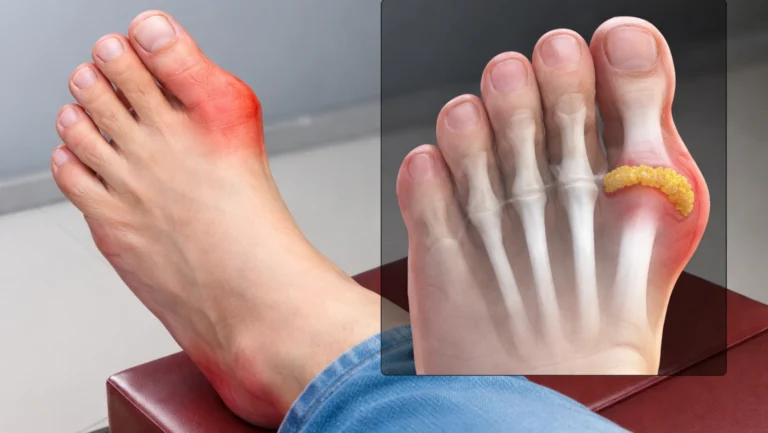
Gout in heel is a form of crystal-induced arthritis where monosodium urate crystals accumulate in the heel joint, triggering sudden, severe inflammation. According to the CDC, gout affects over 8.3 million Americans, and heel involvement, though less discussed than toe gout, accounts for a significant number of misdiagnosed foot pain cases.
Most Americans with heel pain assume plantar fasciitis, but gout in heel follows a completely different pattern. This guide covers causes, symptoms, diagnosis, treatment, and prevention.
What Causes Gout in the Heel
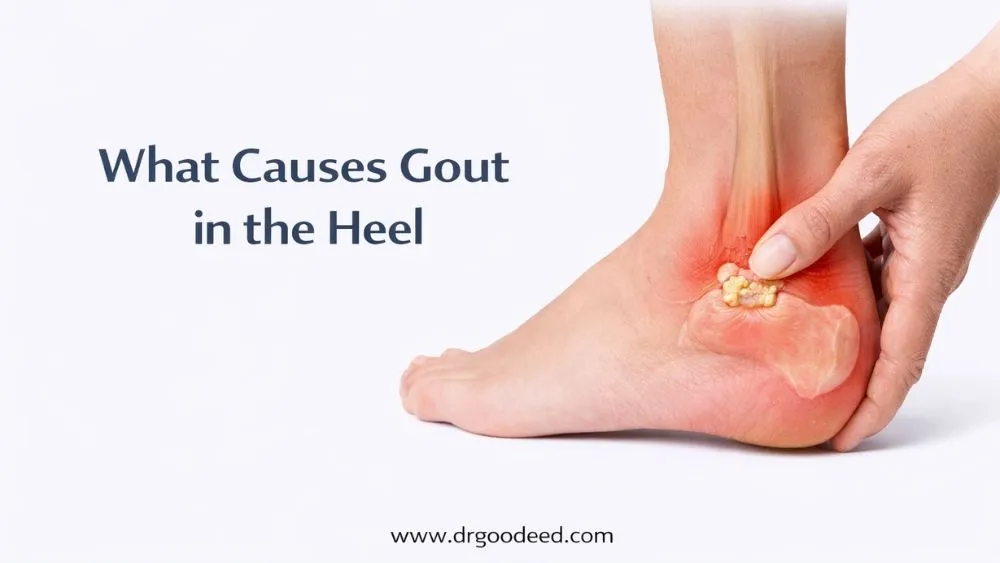
The causes of gout in the heel trace back to chronically elevated uric acid in the blood. When serum uric acid exceeds 6.8 mg/dL, it deposits as sharp crystals inside joints. The heel, specifically the area around the Achilles tendon insertion and subtalar joint, is a common crystal deposition site in people with advanced or long-standing gout.
Uric Acid Buildup in Heel Joint
Uric acid buildup in heel joint happens when kidneys fail to excrete uric acid fast enough. The heel’s lower temperature compared to core body areas speeds up crystal formation. Urate crystals prefer cooler peripheral joints, which is why feet and ankles get hit more often than hips or shoulders. Once crystals settle in the heel’s synovial tissue, any physical stress on the joint, like walking, triggers the immune system’s inflammatory response.
High Purine Diet and Alcohol Intake
Red meat, organ meats, sardines, anchovies, and beer are the main dietary triggers. Fructose-sweetened beverages raise uric acid independently of purine intake. A 2004 study in the New England Journal of Medicine found that men who drank two or more beers daily had a 250% higher risk of gout compared to non-drinkers. Spirits raised risk by 150%. Wine had minimal effect.
Reduced Kidney Function and Dehydration
Kidneys handle about 70% of daily uric acid excretion. Any reduction in kidney function, even early-stage CKD, raises serum uric acid. Dehydration concentrates urine and slows excretion. People in high-heat occupations across the US Sun Belt states, like construction workers in Texas or Arizona, have higher gout incidence partly because of chronic mild dehydration.
Genetics and Metabolic Disorders
Variants in the ABCG2 gene reduce the gut’s ability to excrete uric acid and account for roughly 10% of US gout cases. Metabolic syndrome, which affects nearly 35% of American adults, raises uric acid through insulin resistance. Insulin blocks renal uric acid excretion directly. Hypothyroidism and psoriasis also raise uric acid and increase the risk of gout in people who carry these conditions alongside dietary triggers.
Symptoms of Gout in the Heel
Gout in heel symptoms are intense and come on without warning. The heel becomes one of the most painful areas to bear weight on during a flare, and the inflammation is visible. Recognizing symptoms early speeds up treatment and reduces total flare duration.
Sudden Heel Pain Gout Attack
A sudden heel pain gout attack is the defining symptom. Pain onset happens over 6 to 12 hours, unlike plantar fasciitis which builds gradually over weeks. The heel feels like it is being stabbed with every step. Some patients describe the first sensation as waking up to a burning, throbbing pain that makes putting any foot on the floor impossible.
Warmth in Heel Joint and Redness
Warmth in the heel joint is a common symptom of gout and appears alongside redness, caused by increased blood flow to the inflamed site. The skin over the heel and lower Achilles area turns red or purplish and feels noticeably hotter than the other foot. Pressing lightly on the area produces sharp pain, which rules out conditions like deep vein thrombosis that produce duller tenderness.
Swelling and Tenderness
Swelling in gout in heel cases centers around the back and bottom of the heel. The Achilles tendon area puffs up visibly. Footwear becomes impossible to wear. Even bedsheets touching the heel at night cause intense discomfort.
Difficulty Walking or Putting Weight on Heel
During an active flare, putting full body weight on the heel forces crystal-laden synovial fluid to compress against inflamed tissue. Most people walk on their toes or avoid the affected foot entirely. This compensation gait strains the gout in knee and hip, sometimes causing secondary pain in those joints.
Pain Worse at Night or Early Morning
Core body temperature drops during sleep, which accelerates uric acid crystal formation. Cortisol, the body’s natural anti-inflammatory hormone, hits its lowest levels between midnight and 4 AM. Combined, these two factors mean gout in heel attacks peak during sleeping hours and are typically worst at first waking.
How to Treat Gout in Heel Fast
To treat gout in heel fast in the US, the approach rheumatologists use follows a three-stage protocol: stop the inflammation immediately, manage pain, and prevent the next flare. Starting treatment within 24 hours of the attack cuts recovery time in half.
- NSAIDs: Indomethacin 50mg three times daily or naproxen 500mg twice daily for 5 to 7 days. Available by prescription; indomethacin is the standard rheumatology choice for acute gout.
- Colchicine: 1.2mg at first sign of attack, then 0.6mg one hour later. FDA-approved dosing for acute gout. Works best in the first 12 hours.
- Corticosteroids: Prednisone 30mg to 40mg daily for 5 days is used when NSAIDs are contraindicated, particularly in patients with kidney disease or GI ulcers.
- Ice therapy: Apply a cloth-wrapped ice pack for 20 minutes on, 20 minutes off. Ice reduces prostaglandin activity in inflamed tissue.
- Elevation: Keep the foot raised above hip level to reduce fluid accumulation in the heel area.
- Rest: No weight-bearing activity until swelling visibly decreases, typically 48 to 72 hours.
Do not apply heat during an active flare. Heat increases blood flow and worsens crystal-driven inflammation.
Diagnosis of Heel Gout
Gout in heel is misdiagnosed as plantar fasciitis in a large number of US primary care visits. Accurate diagnosis requires more than a physical exam.
Blood Tests for Uric Acid
Serum uric acid above 6.8 mg/dL supports the diagnosis. However, during an active flare, uric acid levels sometimes fall to normal as crystals move into the joint space. A normal result during a flare does not rule out gout.
Joint Fluid Analysis
Aspiration of the subtalar joint or heel bursa with polarized light microscopy showing negatively birefringent monosodium urate crystals is the diagnostic gold standard. This also rules out septic arthritis in the same procedure.
Imaging
Ultrasound detects the double contour sign over heel cartilage, a urate crystal layer that is highly specific to gout. Dual-energy CT (DECT) maps urate deposits precisely and is available at most academic medical centers in the US. Standard X-rays are normal in early gout but show bone erosions in chronic disease.
Differentiating from Plantar Fasciitis or Heel Spur
Plantar fasciitis pain is worst with the first steps in the morning and improves after a few minutes of walking. Gout in heel pain does not improve with movement; it worsens. Heel spurs show up on X-ray and cause localized bottom-of-heel pain. Gout produces redness and warmth; heel spurs and plantar fasciitis do not.
How Long Does Gout in Heel Last
A treated gout in heel flare resolves in 3 to 7 days with appropriate medication. Without treatment, the flare peaks at day 4 to 5 and fades over 10 to 14 days.
- Colchicine started within 12 hours: significant pain reduction by day 2.
- NSAIDs started within 24 hours: pain drops by day 3.
- No treatment: full resolution takes 2 to 3 weeks, with greater joint damage risk.
Recurrence Risk
Without urate-lowering therapy, 62% of gout patients have a second attack within one year according to research published in Annals of the Rheumatic Diseases. Each recurrence tends to last longer. Keeping serum uric acid below 6 mg/dL stops recurrence almost completely.
Risk Factors for Heel Gout
Gout in heel disproportionately affects American men between 40 and 60. After menopause, women’s risk rises sharply because estrogen previously helped the kidneys excrete uric acid.
Obesity and Sedentary Lifestyle
A BMI above 30 raises serum uric acid because fat tissue produces more uric acid and adipose cells release it into the bloodstream. Sedentary behavior also reduces peripheral circulation, slowing uric acid clearance from joints.
High Purine Diet
Organ meats, red meat eaten more than 5 times weekly, and shellfish raise serum uric acid by 1 to 2 mg/dL above baseline. This alone can push uric acid above the crystallization threshold.
Alcohol Consumption
Beer is the highest-risk drink because it contains both purines and compounds that block renal uric acid clearance simultaneously. Even two beers in one evening raises serum uric acid measurably for up to 24 hours.
Previous Joint Stress or Injury
Prior heel injuries, such as Achilles tendon tears or calcaneal fractures, create scar tissue that urate crystals attach to more easily. Athletes with a history of repetitive heel stress are at higher risk of gout in heel if they also carry elevated uric acid.
Complications of Untreated Heel Gout
Chronic Joint Inflammation
Repeated flares without urate-lowering therapy cause persistent low-grade inflammation that erodes cartilage continuously between attacks.
Tophi Formation in Heel
Hard white uric acid nodules called tophi grow around the Achilles tendon and heel pad. Tophi are visible as lumps under the skin and can rupture, creating open wounds that get infected.
Reduced Mobility and Walking Difficulty
Chronic gout in heel leads to permanent gait changes. Studies show that patients with heel tophi walk 20% to 30% slower and have lower step count per day than matched controls.
Joint Damage
Urate crystals directly damage cartilage and bone. X-rays in chronic cases show “rat bite” erosions at the heel bone edges. This damage is irreversible.
How to Prevent Gout in the Heel
Preventing gout in heel requires keeping serum uric acid below 6 mg/dL long-term. Allopurinol is the first-line urate-lowering drug in the US, starting at 100mg daily and adjusting to 300mg to 600mg based on blood levels tested every 4 to 6 weeks.
- Drink at least 2 to 3 liters of water daily
- Cut out organ meats and limit red meat to twice weekly
- Replace beer with wine if alcohol is consumed
- Aim for a BMI under 25; even a 10-pound weight loss lowers uric acid by about 1 mg/dL
- Test serum uric acid every 6 months if you have had one gout flare
When to See a Doctor
See a doctor within 24 hours if:
- The heel is red, swollen, and hot with fever above 101°F; infection must be ruled out
- Pain does not improve after 48 hours of NSAIDs and ice
- White lumps appear around the heel or Achilles tendon
- This is your second or third flare in a 12-month period; that signals uncontrolled uric acid needing long-term medication
Frequently Asked Questions
Can gout affect the heel?
Yes. Gout in heel occurs in roughly 10% to 15% of gout cases. The subtalar joint and Achilles tendon insertion are the main sites. It is more common in patients who have had untreated gout for 3 or more years.
How do I know if heel pain is gout or plantar fasciitis?
Gout in heel causes visible redness, warmth, and swelling that plantar fasciitis never produces. Plantar fasciitis pain improves after walking for a few minutes. Gout pain stays severe regardless of movement or rest.
Why does heel gout hurt more at night?
Body temperature drops 0.5 to 1 degree Celsius during sleep, which speeds up urate crystal formation in cool peripheral joints like the heel. Cortisol, which suppresses inflammation, also drops to its lowest level between 12 AM and 4 AM.
What is the fastest way to relieve heel gout pain?
Colchicine 1.2mg taken within 12 hours of the sudden heel pain gout attack provides the fastest pharmaceutical relief. Combined with ice packs and elevation, pain typically drops noticeably within 12 to 24 hours.
Can gout in the heel become chronic?
Yes. Without allopurinol or another urate-lowering drug, gout in heel progresses to chronic tophaceous gout in 5 to 10 years. Tophi form around the Achilles tendon, causing permanent stiffness and walking difficulty.
Does walking worsen heel gout?
Yes, walking during an active gout in heel flare forces crystals into compressed tissue, worsening inflammation. Rest the foot completely for the first 48 hours. Resume light walking only after swelling starts to visibly decrease.
What foods trigger heel gout attacks?
Beer is the single highest-risk trigger. Organ meats like liver and kidney, shrimp, scallops, and fructose-sweetened sodas are the next highest. Eating a high-purine meal with beer raises serum uric acid enough to trigger a sudden heel pain gout attack within 12 hours.
Can gout spread from heel to other joints?
Yes. Without urate-lowering therapy, gout in heel spreads to the ankle, knee, and wrist over years as systemic uric acid levels stay elevated. Polyarticular gout affects 4 or more joints simultaneously in advanced cases.
Is heel gout common or rare?
Heel gout is less common than toe gout but more common than most people realize. Among the 8.3 million Americans with gout, heel involvement increases significantly in those with serum uric acid above 9 mg/dL or a gout history longer than 5 years.
Can shoe choice affect heel gout pain?
Yes. During recovery, wide, soft-soled shoes like athletic walking shoes reduce pressure on the inflamed heel. Rigid-soled dress shoes and high heels compress the subtalar joint and worsen pain. Orthotic insoles with heel cushioning reduce impact during the recovery phase.