The traditional Chinese medicine list of herbs, therapies, and diagnostic frameworks forms one of the most comprehensive natural medicine systems in the world, with over 3,000 years of documented clinical use.
The WHO formally recognized Traditional Chinese Medicine (TCM) in the 11th revision of the International Classification of Diseases (ICD-11) in 2019, integrating TCM diagnostic patterns alongside conventional medical codes for the first time.
In the US, over 3.5 million Americans receive acupuncture annually, and TCM herbal products generate over $170 million in annual sales. This guide covers the core disease concepts, five elements theory, complete herb and therapy lists, pain management, gut health protocols, and safety considerations.
Causes of Disease in Traditional Chinese Medicine
The causes of disease in traditional chinese medicine differ fundamentally from the Western biomedical model. TCM does not identify a single pathogen or organ failure as the cause of illness. Instead, it identifies disruptions in the body’s internal energy patterns and its relationship with the external environment.
Qi Deficiency and Stagnation
Qi (pronounced “chee”) is the vital energy that flows through the body along channels called meridians. When Qi runs low, organs lose their functional power; fatigue, poor digestion, and low immunity follow.
When Qi stagnates, it creates localized pain, emotional frustration, and hormonal disruption. Liver Qi stagnation specifically is the TCM diagnosis behind PMS, irritable bowel syndrome, and chronic stress-related headaches.
Yin-Yang Imbalance
Yin represents cooling, moistening, and restorative energy. Yang represents heat, activation, and movement. Disease develops when one dominates the other persistently. Yin deficiency produces night sweats, dry mouth, insomnia, and hot flashes; this pattern appears frequently in perimenopausal women in US TCM clinics. Yang deficiency produces cold limbs, low libido, and fatigue.
External Pathogens (Wind, Heat, Dampness)
TCM classifies external disease triggers as six pathogenic factors: Wind, Cold, Heat, Dampness, Dryness, and Summer Heat. Wind-Heat causes the TCM equivalent of viral upper respiratory infection: sore throat, fever, and rapid pulse. Dampness accumulates from excessive sugar, fried food, and sedentary behavior, producing brain fog, heavy limbs, and digestive bloating.
Organ System Disharmony
TCM organ systems differ from anatomical organs. The TCM “Liver” governs emotion regulation and blood storage. The “Spleen” governs digestion and muscle tone. Each organ has a paired organ, a corresponding emotion, a season, and a color, all connected through the Five Elements framework.
The Five Elements Theory in TCM
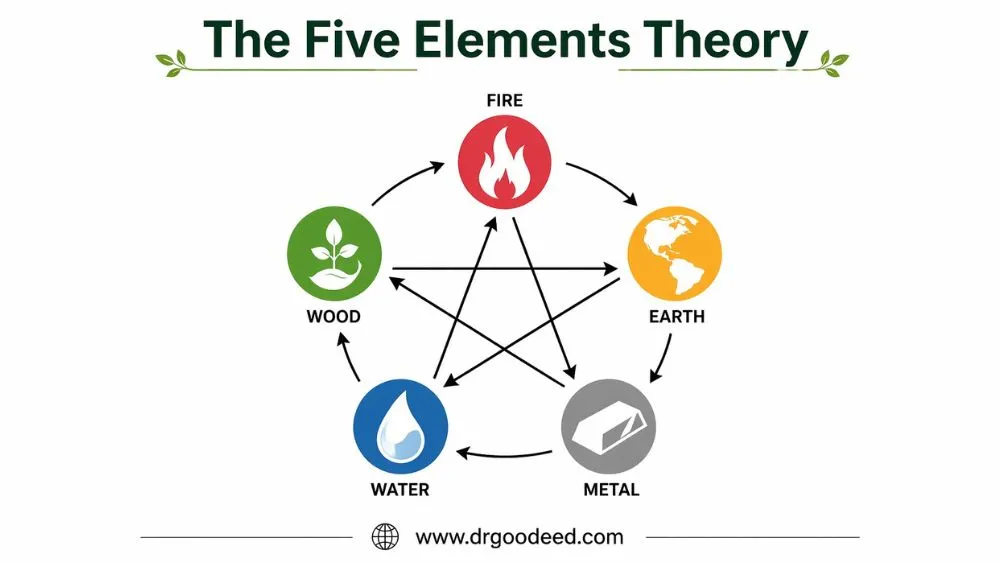
The five-element theory in TCM describes how five natural forces, Wood, Fire, Earth, Metal, and Water, govern body physiology, emotion, and disease progression. Each element maps to specific organs, seasons, and emotional states.
Wood, Fire, Earth, Metal, Water
- Wood: Growth and movement. Associated with Spring.
- Fire: Heat and activation. Associated with Summer.
- Earth: Nourishment and stability. Associated with Late Summer.
- Metal: Structure and boundaries. Associated with Autumn.
- Water: Storage and restoration. Associated with Winter.
Organ Connections
| Element | Yin Organ | Yang Organ | Emotion | Season |
| Wood | Liver | Gallbladder | Anger | Spring |
| Fire | Heart | Small intestine | Joy | Summer |
| Earth | Spleen | Stomach | Worry | Late Summer |
| Metal | Lung | Large intestine | Grief | Autumn |
| Water | Kidney | Bladder | Fear | Winter |
How Imbalance Leads to Disease
Each element supports and controls adjacent elements in a cycle. When one element weakens, it fails to nourish the next and cannot control the one it is supposed to restrain.
A weakened Earth (Spleen) fails to produce adequate Qi, which depletes Metal (Lung) and allows Wood (Liver) to over-dominate, producing digestive weakness alongside anxiety and tension headaches simultaneously.
Types of Traditional Chinese Medicine Therapies
The full traditional Chinese medicine list of therapies includes both physical and herbal interventions, each targeting a different aspect of Qi flow, organ function, and pathogen clearance.
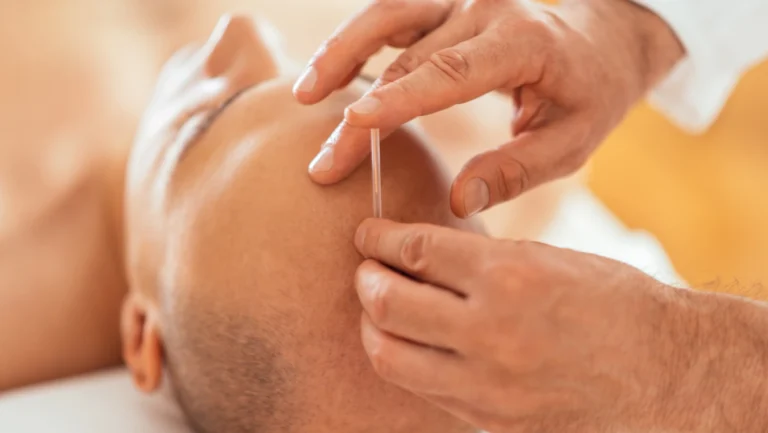
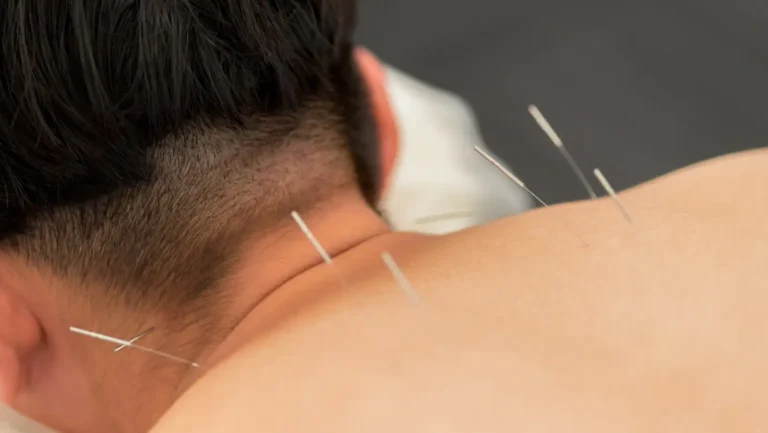
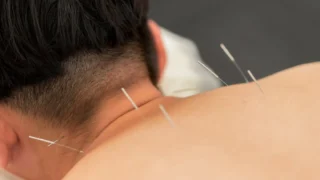
Acupuncture
Fine needles inserted at specific meridian points regulate Qi flow. The US National Institutes of Health (NIH) confirmed acupuncture’s effectiveness for chronic low back pain, neck pain, osteoarthritis, and chemotherapy-induced nausea. Over 35,000 licensed acupuncturists practice in the US.
Moxibustion
Dried Mugwort (Artemisia vulgaris) burns near acupuncture points to warm channels and dispel Cold and Dampness. It is used specifically for Cold-pattern conditions: cold limbs, digestive weakness, and breech presentation in pregnancy. A Cochrane Review confirmed moxibustion significantly increases the rate of cephalic (head-down) fetal repositioning before delivery.
Cupping Therapy
Glass or silicone cups create suction on the skin. This draws stagnant blood to the surface, improves local circulation, and releases tight fascia. Athletes like US Olympic swimmer Michael Phelps brought cupping into global awareness after the 2016 Rio Olympics.
Tui Na Massage
Tui Na is a therapeutic Chinese massage that uses specific hand techniques to move Qi through meridians. It combines compression, rolling, and joint mobilization. It is particularly effective for musculoskeletal pain, frozen shoulder, and cervical spondylosis.
Chinese Herbal Medicine
Single herbs and multi-herb formulas treat internal organ imbalances. Classical formulas like Si Jun Zi Tang (Four Gentlemen Decoction) strengthen Spleen Qi. Xiao Chai Hu Tang treats Liver-Spleen disharmony. Formulas always contain a chief herb, a deputy herb, an assistant, and an envoy herb to direct the formula to the correct organ.
Tai Chi and Qigong
Tai Chi and Qigong are moving meditation practices that cultivate and regulate Qi. A 2012 meta-analysis in PLOS ONE confirmed Tai Chi reduces blood pressure by an average of 15.6 mm Hg systolic and improves balance, reducing fall risk in adults over 65 by 43%.
Top 10 Traditional Chinese Medicine Herbs List
The top 10 traditional Chinese medicine herbs list includes the most clinically studied and widely used herbs in TCM practice globally.
Ginseng (Ren Shen): Energy and Immunity
Panax ginseng improves Qi in the Heart, Lung, and Spleen simultaneously. Ginsenosides reduce cortisol, improve cognitive performance, and stimulate natural killer cell activity. A 2020 meta-analysis in Medicine confirmed ginseng improved fatigue outcomes across 10 randomized controlled trials.
Astragalus (Huang Qi): Immune Support
Astragalus membranaceus is the primary herb for Wei Qi, which is the defensive energy that protects against external pathogens. Polysaccharides in Astragalus increase CD4+ T-cell counts and NK cell activity. The Memorial Sloan Kettering Cancer Center lists Astragalus as a studied immune-supportive herb for oncology patients.
Licorice Root (Gan Cao): Harmonizing Herb
Gan Cao appears in roughly 60% of classical TCM formulas as an envoy herb that moderates the actions of other herbs and protects the digestive tract. Glycyrrhizin in licorice has documented anti-inflammatory and antiviral properties. Long-term use above 6g daily raises blood pressure due to cortisol-modulating effects.
Ginger (Sheng Jiang): Digestion and Inflammation
Fresh ginger disperses Cold from the Stomach and Lungs. It reduces nausea (confirmed in pregnancy and chemotherapy contexts), stimulates gastric acid secretion, and inhibits prostaglandin synthesis. Dry ginger (Gan Jiang) is a stronger Yang tonic used for chronic cold-pattern digestive disorders.
Reishi Mushroom (Ling Zhi): Immunity and Stress
Reishi is a Shen tonic, meaning it calms the mind and strengthens the Heart. Beta-glucans in Reishi modulate the immune system bidirectionally, calming autoimmune overactivity and stimulating deficient immune responses. The National Cancer Institute includes Reishi in its clinical trials database.
Dang Gui: Blood Circulation and Women’s Health
Dang Gui (Angelica sinensis) is the primary Blood tonic in TCM. It nourishes Blood, regulates menstruation, and improves circulation. Ferulic acid in Dang Gui inhibits platelet aggregation and reduces uterine cramping. It is the central herb in most classical formulas for irregular periods, PMS, and postpartum recovery.
Goji Berries (Gou Qi Zi): Antioxidant Support
Goji berries tonify Liver and Kidney Yin and improve eyesight in TCM. Zeaxanthin in Goji berries reduces macular degeneration risk. A 2011 study in Optometry and Vision Science confirmed Goji supplementation increased plasma zeaxanthin levels by 26% over 90 days.
Schisandra (Wu Wei Zi): Liver and Stress Support
Schisandra’s name means “five-flavor fruit” because it contains all five TCM tastes in one berry. It is an adaptogen that protects liver cells from oxidative damage and reduces cortisol response to physical and mental stress. Russian Olympic athletes used Schisandra during training for its endurance-enhancing properties in the 1950s and 1960s.
Atractylodes (Bai Zhu): Digestion and Metabolism
Bai Zhu strengthens Spleen Qi and dries Dampness. It is the primary herb for TCM digestive weakness characterized by loose stools, fatigue after eating, and heavy limbs. Atractylolide compounds in Bai Zhu improve gastric motility and reduce intestinal inflammation.
Jujube (Suan Zao Ren): Sleep and Calming
Suan Zao Ren (sour jujube seed) nourishes Heart Blood and calms the Shen (mind). It reduces sleep latency and improves sleep quality without causing morning grogginess. A 2020 study in Phytomedicine confirmed Suan Zao Ren extract reduced insomnia severity scores significantly over 4 weeks.
Herbal Remedies in Chinese Medicine for Immunity
Herbal remedies in Chinese medicine for immunity work through three mechanisms: strengthening Wei Qi (defensive energy), clearing pathogens already present, and restoring organ function after illness.
Qi Tonics for Immune Strength
- Astragalus (Huang Qi): increases T-cell and NK cell counts
- Codonopsis (Dang Shen): gentler Qi tonic for prolonged use
- White Atractylodes (Bai Zhu): strengthens Spleen Qi to build daily immune reserves
Adaptogenic Herbs
Adaptogens in TCM regulate the HPA axis response to stress. Chronic stress is the most consistent predictor of immune suppression. Schisandra, Eleuthero (Ci Wu Jia), and Reishi are the three primary TCM adaptogens used in US integrative clinics.
Seasonal Immune Support Formulas
Yu Ping Feng San (Jade Windscreen Formula) is a three-herb formula of Astragalus, Atractylodes, and Siler root used specifically as a preventive during cold and flu season. A 2007 Cochrane Protocol identified it as one of the most studied TCM immune formulas, with multiple Chinese RCTs showing reduced upper respiratory infection frequency.
How TCM Classifies Herbs
TCM herb classification uses four criteria that determine which conditions each herb treats and how it interacts with other herbs in a formula.
Temperature (Hot, Warm, Cool, Cold)
Cold herbs (like Huang Lian/Coptis) clear Heat and inflammation. Hot herbs (like Fu Zi/Aconite) warm Cold-pattern conditions. Using a Cold herb for a Cold-pattern patient worsens symptoms dramatically.
Taste (Sweet, Bitter, Sour, Pungent, Salty)
Sweet herbs tonify and slow. Bitter herbs drain Heat and dry Dampness. Pungent herbs disperse and move Qi. Sour herbs consolidate and astringe. Salty herbs soften hardness and drain downward. A single herb’s taste combination tells the TCM practitioner which organ it targets and what action it performs.
Meridians and Organ Targeting
Each herb enters specific meridians. Ginger enters the Lung, Spleen, and Stomach meridians. This explains why it treats both respiratory infections and digestive upset simultaneously.
TCM for Pain Management Therapies
TCM for pain management therapies treats pain as Qi and Blood stagnation. Where there is free flow, there is no pain. Where there is obstruction, there is pain. This single principle guides all TCM pain interventions.
Acupuncture for Chronic Pain
The US National Institutes of Health funded an individual patient data meta-analysis (published in JAMA Internal Medicine, 2018) covering 20,827 patients across 39 trials. Acupuncture produced statistically significant pain relief for chronic back pain, neck pain, osteoarthritis, and headache, with effects persisting 12 months after treatment ended.
Cupping for Muscle Tension
Cupping separates fascia layers, increases local circulation, and draws inflammatory metabolites to the skin surface for clearance. Sports medicine teams at multiple US professional football clubs use cupping as a standard recovery tool.
Herbal Formulas for Inflammation
Juan Bi Tang (Remove Painful Obstruction Decoction) contains herbs that reduce Wind-Damp joint inflammation. Du Huo Ji Sheng Wan targets Kidney-deficient low back and knee pain. Yan Hu Suo (Corydalis) contains THP, an alkaloid that blocks dopamine receptors involved in pain signaling.
TCM Approach to Arthritis and Joint Pain
Bi Syndrome (painful obstruction) is the TCM classification for arthritis. Wind-Bi causes migratory joint pain. Cold-Bi causes fixed, severe joint pain that worsens in winter. Damp-Bi causes heavy, swollen joints. Treatment selects herbs matching the specific Bi pattern rather than using the same formula for all arthritis patients.
TCM for Digestion and Gut Health
Strengthening Spleen and Stomach
The Spleen is the TCM center of digestion. Spleen Qi deficiency produces loose stools, bloating, fatigue after eating, and weight gain from fluid retention. Si Jun Zi Tang (Four Gentlemen) and Liu Jun Zi Tang (Six Gentlemen) are the standard classical formulas for Spleen Qi deficiency.
Herbs for Bloating and Indigestion
- Chen Pi (aged tangerine peel): moves Qi in the stomach and reduces food stagnation
- Sha Ren (cardamom): warms the Spleen and reduces nausea
- Lai Fu Zi (radish seed): reduces food stagnation and gas
- Ban Xia (pinellia): reduces vomiting and phlegm accumulation in the stomach
Role of Diet in TCM
TCM classifies all foods by temperature and taste. Cold foods (raw salads, iced drinks, cold dairy) weaken Spleen Yang over time. Warm, cooked foods support Spleen Qi. Eating at irregular times, skipping meals, and working through lunch are specific habits TCM practitioners identify as direct causes of long-term digestive weakness in US patients.
When to Use Traditional Chinese Medicine
TCM works best for chronic conditions that conventional medicine manages but does not resolve. Chronic fatigue, functional digestive disorders, hormonal imbalances, stress-related insomnia, and recurring respiratory infections all respond well to the traditional chinese medicine list of herbal and physical therapies.
For acute emergencies including heart attack, stroke, appendicitis, and severe infection, conventional emergency medicine is the appropriate first-line intervention. TCM provides the best outcomes when used alongside, not instead of, conventional care for serious diagnosed conditions.
Frequently Asked Questions
Is traditional Chinese medicine scientifically proven?
Yes, for specific conditions. Acupuncture for chronic pain has Level 1A evidence from a 20,827-patient meta-analysis published in JAMA Internal Medicine. Artemisinin, derived from TCM herb Qing Hao, won the 2015 Nobel Prize in Medicine for malaria treatment. The traditional chinese medicine list of evidence-backed therapies grows annually.
Can TCM boost immunity?
Yes. Astragalus (Huang Qi) at 15g to 30g daily increases CD4+ T-cells and NK cell activity within 4 to 8 weeks. The herbal remedies in Chinese medicine for immunity formula Yu Ping Feng San reduced acute respiratory infection frequency by 40% versus placebo in a Chinese multicenter trial covering 1,200 patients.
How does acupuncture relieve pain?
Acupuncture and dry needles stimulate A-delta and C nerve fibers, triggering endorphin and enkephalin release in the spinal cord and brainstem. This activates the descending pain inhibition pathway, the same system targeted by opioid medications. Functional MRI studies confirm acupuncture changes brain activity in pain-processing regions within 30 seconds of needle insertion.
Are Chinese herbs safe for long-term use?
Yes, for most classical formulas at standard doses. Gan Cao (licorice) above 6g daily raises blood pressure from aldosterone-like activity. Fu Zi (aconite) requires precise preparation to eliminate cardiotoxic alkaloids. Always use formulas from licensed TCM practitioners or GMP-certified brands like Evergreen Herbs or KPC Herbs in the US.
What is Qi in Chinese medicine?
Qi is the functional energy that powers all physiological processes in TCM. It is not mystical; it maps onto measurable concepts including mitochondrial ATP production, neural signaling, and organ metabolism. Deficient Qi corresponds clinically to fatigue, immune weakness, and organ hypofunction. Stagnant Qi corresponds to pain, emotional tension, and impaired circulation.
Can TCM treat chronic diseases?
Yes, for management and symptom reduction. The traditional Chinese medicine list of conditions with clinical evidence includes chronic pain, IBS, insomnia, menopausal symptoms, and chemotherapy side effects. TCM does not reverse structural damage from advanced diabetes or cardiovascular disease but measurably improves quality of life and symptom burden.
How long does TCM take to work?
Acute conditions like cold, digestive upset, or pain respond within 1 to 3 sessions or 3 to 7 days of herbal use. Chronic conditions like hormonal imbalance, chronic fatigue, or insomnia require 8 to 12 weeks of consistent treatment. The five-element theory in TCM guides practitioners in predicting which conditions respond faster based on organ involvement.
What is the difference between Ayurveda and TCM?
Both are 3,000-year-old systems that treat root causes over symptoms. Ayurveda uses three doshas (Vata, Pitta, Kapha) for diagnosis. TCM uses Qi, Yin-Yang, and Five Elements. Ayurveda prescribes single herbs more often. TCM relies primarily on multi-herb formulas targeting specific meridian patterns. Both are recognized by the WHO under traditional medicine frameworks.
Do TCM herbs have side effects?
Yes. Huang Lian (Coptis) causes GI irritation at high doses. Da Huang (rhubarb root) causes diarrhea and electrolyte loss if overused. Some traditional Chinese medicine list herbs like Aristolochic acid-containing herbs (Guan Mu Tong) are banned in the US due to kidney toxicity. Always source herbs from licensed practitioners or NSF-certified US suppliers.










Leave a Comment