Stress can cause kidney stones, and the connection runs through specific hormonal and behavioral pathways. Chronic stress triggers cortisol and adrenaline release, which alters how the kidneys filter minerals, concentrate urine, and regulate calcium excretion. About 1 in 10 Americans develops kidney stones in their lifetime, according to the National Kidney Foundation, and psychological stress is an underrecognized contributor.
How Stress Affects the Urinary System
Stress and urinary system problems start with the same hormonal chain that affects every other organ system. Cortisol and adrenaline don’t only raise heart rate and blood pressure. They directly alter how the kidneys handle calcium, sodium, and oxalate, the three primary building blocks of kidney stones.
Hormonal Changes Impacting Kidney Function
Cortisol increases calcium excretion through the urine. During acute stress, the adrenal glands release cortisol, which signals the kidneys to flush more calcium than normal. This is measurable. A study published in Kidney International confirmed that hypercortisolism, a state of excess cortisol, directly elevates urinary calcium levels.
When calcium levels in urine exceed what the kidneys can dissolve, calcium oxalate crystals begin forming. Those crystals are the most common kidney stone type, accounting for about 80% of all cases in the US.
Altered Urine Concentration
Adrenaline diverts blood flow away from the kidneys toward muscles during the stress response. Reduced blood flow to the kidneys causes them to produce less urine and make that urine more concentrated. Concentrated urine holds more dissolved minerals per unit of liquid. When mineral concentration crosses a saturation point, crystals form. The kidneys cannot dissolve what is already supersaturated.
Increased Mineral Buildup Risk
Chronic stress also suppresses the production of citrate, a natural compound the kidneys release that prevents crystal formation by binding to calcium. Research published in the Journal of Urology found significantly lower urinary citrate levels in patients with recurrent kidney stones compared to stone-free controls. Stress-driven cortisol suppression of citrate production removes the kidneys’ primary defense against stone formation.
Reduced Fluid Intake Stress Kidney Stones
Reduced fluid intake stress kidney stones is one of the most direct and least discussed pathways. When people are under stress, they forget to drink water. They skip meals. They drink coffee and alcohol instead, both of which are diuretics that increase fluid loss. This behavioral pattern concentrates the urine rapidly.
Dehydration During Stress
The kidneys need roughly 2.5 liters of urine output daily to keep minerals dissolved and prevent crystal formation. Most US adults under moderate stress produce significantly less than this. Dehydration during high-stress periods, like exam weeks, high-stakes work projects, or family crises, reduces urine output fast. The kidneys respond by reabsorbing more water and making the remaining urine extremely concentrated.
Concentrated Urine Formation
Urine concentration is measured by specific gravity. Normal urine sits between 1.002 and 1.030. When specific gravity consistently stays above 1.025 due to low fluid intake, the risk of crystal formation increases sharply. Dark yellow or amber urine is a visible sign that concentration has reached a dangerous level for stone-prone individuals.
Higher Chance of Crystal Formation
Calcium, oxalate, and uric acid all become less soluble as urine concentration increases. The relationship is not linear; doubling the concentration more than doubles the crystal formation risk due to the physics of supersaturation. This is why stress increase risk of kidney stones has a clear yes answer: stress reduces fluid intake at precisely the moment cortisol is already pushing more calcium and less citrate into the urine.
Stress and Urinary System Problems
Stress and urinary system problems extend beyond stone formation. Chronic stress changes urination patterns in ways that compound kidney stone risk over time.
Changes in Urination Patterns
Stress activates the sympathetic nervous system, which suppresses normal bladder signaling. Many stressed people urinate less frequently throughout the day. Less frequent urination means minerals sit in the renal collecting system longer. Extended contact time between supersaturated urine and kidney tissue increases the chance of crystals adhering to the renal papillae, the primary location where stones begin forming.
Increased Risk of Urinary Imbalance
Chronic stress elevates urinary sodium excretion. High sodium in urine draws more calcium out of the body alongside it, a process called sodium-calcium cotransport. Every 100 mmol increase in urinary sodium increases urinary calcium by approximately 1 mmol. For people already genetically prone to calcium oxalate stones, this sodium effect during stress is a significant accelerant.
Impact on Kidney Filtration
The kidneys filter approximately 180 liters of blood daily. Stress-driven vasoconstriction, the narrowing of blood vessels, reduces kidney filtration rate. A reduced glomerular filtration rate (GFR) means the kidneys clear waste products more slowly. This slower clearance allows oxalate and uric acid to accumulate in the renal tubules, increasing stone-forming potential.
Other Factors That Combine With Stress to Cause Stones
Stress increases the risk of kidney stones enough on its own. More often, it amplifies existing risk factors that were already present. These combinations produce the highest kidney stone recurrence rates.
High Salt and Processed Food Intake
Stressed Americans eat more processed food. Processed food is high in sodium, phosphoric acid (from sodas), and animal protein, all of which increase urinary calcium and uric acid excretion. A diet regularly exceeding 2,300 mg of sodium daily raises kidney stone risk independent of stress. Combined with stress-elevated cortisol, the effect compounds.
Low Water Consumption
The National Kidney Foundation recommends 2.5 to 3 liters of fluid daily for adults with a history of kidney stones. Most US adults consume significantly less, especially under stress. This single factor, consistent low fluid intake, is the most modifiable and most impactful risk factor for kidney stone recurrence.
Sedentary Lifestyle
Prolonged sitting reduces bone loading. Unloaded bones release calcium into the bloodstream, which the kidneys then excrete into the urine. Sedentary behavior during high-stress periods, like remote work with minimal movement, contributes to hypercalciuria through this mechanism.
Genetic Predisposition
People with a family history of kidney stones, primary hyperoxaluria, or cystinuria face dramatically elevated baseline risk. Stress does not cause these genetic conditions, but it activates the hormonal environment that makes stone formation much more likely for people who carry these predispositions.
Symptoms of Kidney Stones
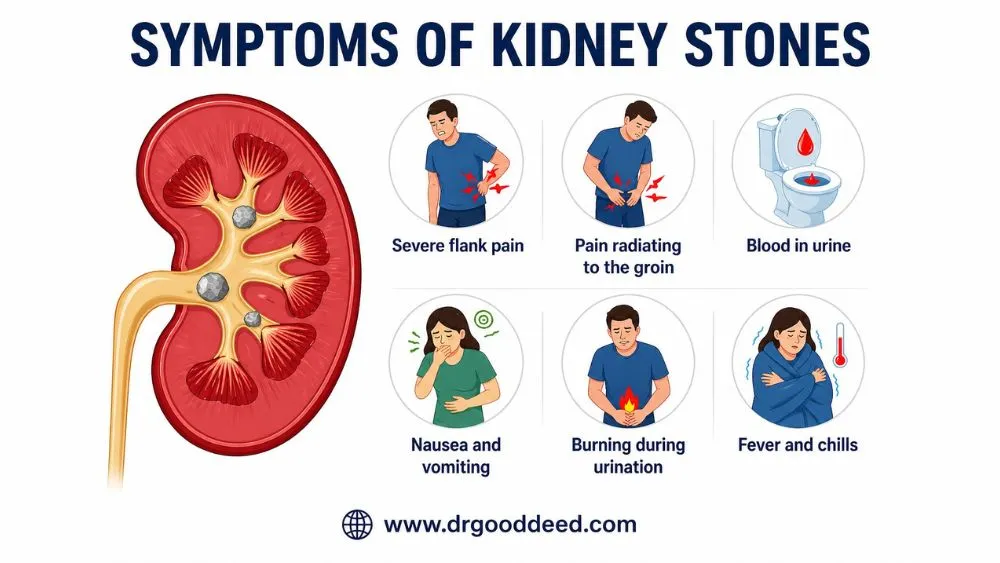
Stress can cause kidney stones severe enough to produce serious symptoms. These are the specific signs that a stone has formed and may be moving through the urinary tract.
- Severe flank pain: Sharp, cramping pain on one side of the back below the ribs, often described as the worst pain experienced. It comes in waves as the stone moves through the ureter
- Pain radiating to the groin: As the stone moves down toward the bladder, pain shifts from the back to the lower abdomen and groin
- Blood in urine (hematuria): Pink, red, or brown urine indicates the stone is scraping the ureter lining. This is visible in about 80% of kidney stone cases
- Nausea and vomiting: The vagus nerve connects the ureter to the digestive system; ureteral pain triggers nausea reflexively
- Frequent urge to urinate: A stone near the bladder creates a sensation of needing to urinate constantly, even when the bladder is nearly empty
- Burning during urination: Indicates the stone has reached the lower ureter or urethra
- Fever and chills: Signals infection behind the stone; this is a medical emergency requiring immediate care
How to Prevent Kidney Stones During Stress
Preventing kidney stones during stress requires targeting both the hormonal mechanism and the behavioral patterns stress creates. General advice about “drinking more water” misses the cortisol and citrate components.
- Drink enough water to produce at least 2 liters of clear urine daily; set phone reminders during high-stress periods because thirst signals become unreliable under chronic stress
- Add fresh lemon juice to water daily; lemon juice is high in citric acid, which raises urinary citrate and directly inhibits calcium oxalate crystal formation by approximately 30 to 40% in clinical studies
- Avoid energy drinks and sodas during stressful periods; phosphoric acid in colas lowers urinary pH and promotes uric acid stone formation
- Practice stress-reduction techniques that reduce cortisol, specifically aerobic exercise and diaphragmatic breathing, both of which lower cortisol measurably within one session
- Limit sodium to under 2,300 mg daily; reading labels on processed food reveals that most single-serving items already contain 600 to 900 mg
- Weigh yourself weekly; sudden weight gain during stress (from retained sodium and inflammation) correlates with urinary mineral changes that increase stone risk
Diet Changes for Kidney Stone Prevention
Diet changes for kidney stone prevention are the most controllable intervention. Specific dietary adjustments reduce stone risk by 40 to 50% in people with recurrent stones, based on data from long-term dietary trials.
Reducing Salt Intake
Target under 1,500 mg of sodium daily for anyone with a history of calcium stones. Each gram of sodium reduction lowers urinary calcium excretion by approximately 10 mg per day. Over months, this reduction measurably decreases crystallization risk.
Limiting Oxalate-Rich Foods
Calcium oxalate stones (the most common type) form when oxalate from food binds to calcium in the kidneys. High-oxalate foods include spinach, almonds, rhubarb, beets, and chocolate. Limiting these foods, particularly spinach and almonds, reduces urinary oxalate by 15 to 25% in stone-prone individuals.
Adequate Calcium Intake
Most people with kidney stones are told to avoid calcium. This is incorrect for calcium oxalate stones. Dietary calcium (from food, not supplements) binds oxalate in the gut before it reaches the kidneys.
The DASH diet, which includes 1,000 to 1,200 mg of calcium daily from dairy and plant sources, reduces kidney stone risk by 40 to 45% compared to low-calcium diets. Calcium supplements, however, taken without food, increase stone risk.
Increasing Fluid-Rich Foods
Cucumbers, watermelon, oranges, celery, and strawberries all contribute significant water content to daily intake. Including these foods during stress periods raises fluid intake passively, even when someone forgets to drink water actively. Watermelon and citrus fruits also contain citrate, adding the crystal-inhibiting benefit on top of hydration.
FAQs
Can stress cause kidney stones?
Yes. Stress can cause kidney stones through cortisol-driven calcium excretion, suppressed urinary citrate production, dehydration from reduced fluid intake, and sodium-calcium cotransport effects. These four mechanisms operate simultaneously during chronic stress, creating the exact urinary chemistry that causes calcium oxalate crystals to form.
Does stress increase risk of kidney stones?
Yes. Stress increases the risk of kidney stones by raising urinary calcium, reducing citrate (the kidneys’ natural crystal inhibitor), concentrating urine through dehydration, and accelerating mineral buildup. The risk compounds when stress combines with high sodium diet, low water intake, or genetic predisposition to hypercalciuria.
Can stress worsen kidney stone pain?
Yes. Cortisol sensitizes pain receptors in the ureter during stress. The same stone produces more intense pain in a chronically stressed person than in a physiologically calm one, because stress-driven central sensitization amplifies pain signal intensity. Adrenaline also causes ureteral spasm, which intensifies cramping around a moving stone.
Why do kidney stones recur?
Kidney stones recur in 50% of patients within 5 years without dietary change, based on National Kidney Foundation data. Recurrence happens because the underlying urinary chemistry, low citrate, high calcium, low fluid output, or high oxalate, remains unchanged after the first stone passes. Chronic stress maintains these conditions persistently.
When should I see a doctor for kidney stones?
See a doctor immediately if flank or groin pain accompanies fever above 101°F, chills, inability to urinate, or blood in urine with vomiting. These signs indicate infection or urinary obstruction behind the stone, both of which require emergency treatment. Pain alone without fever warrants same-day urgent care evaluation.