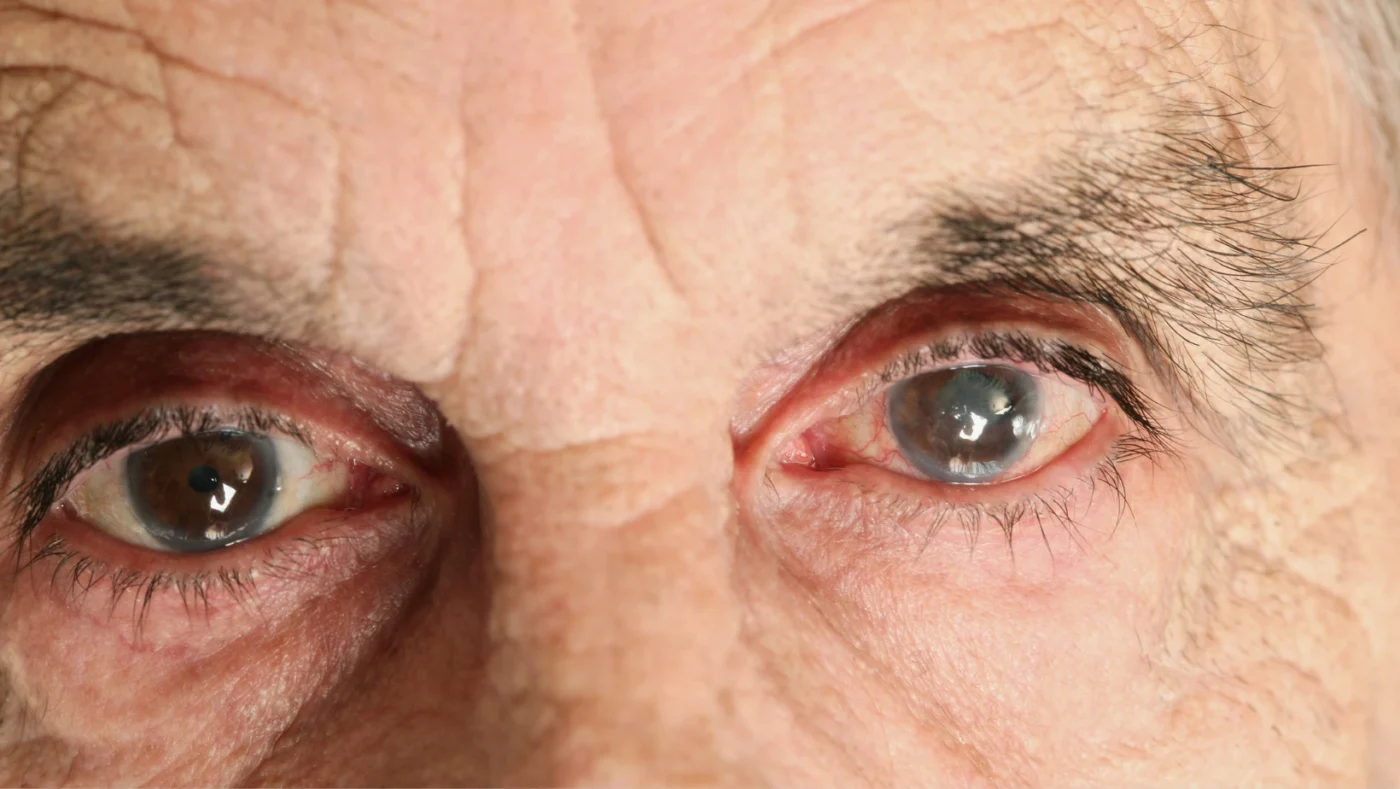
An eye stroke is a sudden blockage of blood flow to the retina, the light-sensitive tissue at the back of the eye that sends visual information to the brain. Clinically classified as Retinal Artery Occlusion (RAO) or Retinal Vein Occlusion (RVO) under ICD-10 codes H34 and H34.8, this condition causes vision loss that ranges from partial dimming to complete blackout in the affected eye, often within minutes.
This guide covers how eye stroke affects vision, its causes, the diabetes connection most articles underexplain, treatment options, and when to treat it as a medical emergency.
How Eye Stroke Affects Vision
Eye stroke affects vision, depending on which blood vessel is blocked and how completely the blockage cuts off oxygen. The retina consumes more oxygen per unit weight than any other tissue in the body, including brain tissue. A blockage lasting 90 minutes or more causes irreversible retinal cell death, per research in Archives of Ophthalmology.
Retina’s Dependence on Blood Supply
The retina receives blood through two separate systems: the central retinal artery (which branches from the ophthalmic artery) and the retinal veins that drain used blood back out. A blockage in either direction starves retinal cells of oxygen or causes them to flood with backed-up blood. Both outcomes kill photoreceptor cells fast.
Oxygen Deprivation and Tissue Damage
Retinal neurons begin dying within 4-6 minutes of complete oxygen cutoff. This is faster than most brain regions during a standard stroke. Partial blockages cause slower damage but still produce measurable vision loss within hours. Dead retinal cells do not regenerate.
Rapid Vision Loss Due to Blocked Arteries or Veins
Central retinal artery occlusion (CRAO) produces the most severe outcome: sudden, complete, painless vision loss in one eye, typically described by patients as a “black curtain” falling over vision. Branch retinal artery occlusion (BRAO) blocks a smaller vessel and causes partial vision loss, often affecting only a section of the visual field.
Sudden Vision Loss in One Eye Stroke
Sudden vision loss in one eye stroke is the defining symptom. It requires emergency evaluation, not a next-week ophthalmology appointment.
Partial or Complete Vision Loss
CRAO causes complete vision loss in the affected eye within seconds to minutes. BRAO and retinal vein occlusions typically cause partial loss, where patients lose a quadrant or half of their visual field. A 2020 study in JAMA Ophthalmology found that 74% of CRAO patients had visual acuity of 20/400 or worse at presentation.
Blurred or Dim Vision
Retinal vein occlusion sometimes presents as blurring rather than blackout. The blocked vein causes blood to leak into the retina, producing swelling (macular edema) that distorts central vision. Patients often describe it as looking through frosted glass.
Shadow or Dark Area in Vision
A dark or grey shadow covering part of the visual field, called a scotoma, is the classic presentation of branch artery or vein occlusion. The shadow location corresponds directly to the area of retina that lost blood supply. It does not move when the eye moves.
Causes of Eye Stroke

An eye stroke shares many of the same root causes as a brain stroke. The retinal blood vessels are part of the same vascular system.
Blood Clots Blocking Retinal Vessels
Emboli (small clots or debris) travel from the heart or carotid artery and lodge in the central retinal artery. Cholesterol plaques, called Hollenhorst plaques, are visible on fundus examination and indicate a systemic embolic source. Their presence in a retinal artery is a strong predictor of future brain stroke.
Atherosclerosis (Narrowed Arteries)
Fatty plaque buildup inside arterial walls narrows the central retinal artery over time. When the artery narrows enough, even a small clot can create a complete blockage. Atherosclerosis is the underlying cause in the majority of CRAO cases in adults over 60.
Diabetes and Retinal Blood Flow Issues
Diabetes and retinal blood flow issues create a distinct pathway to eye stroke. Chronically elevated blood glucose damages the walls of retinal capillaries, making them leak, swell, and close off progressively. This process, called diabetic retinopathy, affects approximately 34% of diabetic adults in the US per the CDC.
High Blood Pressure and Cholesterol
Uncontrolled hypertension damages vessel walls and accelerates plaque formation. A blood pressure reading consistently above 140/90 mmHg doubles the risk of retinal vein occlusion, per data from the British Journal of Ophthalmology.
Diabetes and Retinal Blood Flow Issues
Diabetes and retinal blood flow issues deserve a separate section because the mechanism differs from standard arterial blockage, and most articles treat diabetes as just another bullet point in a risk factor list.
Damage to Blood Vessels in the Eye
High blood glucose triggers a process called advanced glycation end-product (AGE) formation, which stiffens and thickens the walls of small retinal blood vessels. These thickened walls reduce the vessel’s internal diameter without any clot formation. The retina receives less blood even when no blockage exists.
Reduced Circulation to Retina
As diabetic retinopathy progresses, small retinal capillaries begin closing permanently. The retina compensates by growing new blood vessels through a process called neovascularization. These new vessels are fragile and prone to bleeding, which worsens vision and raises eye stroke risk significantly.
Increased Risk of Blockage
Diabetic patients with retinopathy have a 3.4 times higher risk of retinal vein occlusion compared to non-diabetic adults, per the American Journal of Ophthalmology. Blood pressure control directly affects this risk; HbA1c levels above 8% correlate with faster retinal vessel deterioration.
Other Risk Factors for Eye Stroke
An eye stroke becomes more likely when multiple risk factors exist together. Each additional risk factor compounds the probability of blockage.
- Age above 60: Retinal artery occlusion is rare under 40 and increases sharply after 60
- Glaucoma: Elevated intraocular pressure reduces blood flow to the optic nerve and central retinal vein, increasing vein occlusion risk by 2.3 times
- Blood clotting disorders: Factor V Leiden mutation and antiphospholipid syndrome increase clot formation in retinal vessels
- Oral contraceptive use in women with migraines: This combination raises stroke and retinal occlusion risk, confirmed by multiple cardiovascular studies
- Obstructive sleep apnea: Repeated nighttime oxygen drops stress retinal blood vessels over time
How to Restore Vision After Eye Stroke
Restoring vision after eye stroke depends entirely on which vessel is affected, how long the blockage lasted before treatment, and whether underlying conditions are managed. Full recovery is uncommon. Partial recovery is realistic with fast intervention.
Immediate Medical Treatment
CRAO is a medical emergency with a treatment window of under 4 hours. Ocular massage (applying rhythmic pressure to the eye to dislodge an embolus) and anterior chamber paracentesis (removing a small amount of eye fluid to reduce pressure) are two interventions used in emergency settings. Neither restores vision consistently, but both are attempted when the patient arrives within the window.
Medications to Reduce Pressure or Improve Flow
Intravitreal anti-VEGF injections (bevacizumab or ranibizumab) are the standard treatment for retinal vein occlusion with macular edema. These injections reduce retinal swelling and stop abnormal vessel growth. Patients typically receive monthly injections for 3-6 months initially.
Managing Underlying Conditions
Controlling blood pressure, blood sugar, and cholesterol does not reverse existing retinal damage but prevents the second eye from experiencing the same event. Roughly 16% of patients with a retinal artery occlusion in one eye develop a brain stroke within 3 months without vascular intervention, per the New England Journal of Medicine.
Why Immediate Treatment Matters
Retinal tissue begins dying within 4-6 minutes of complete artery blockage. A delay of even 2-3 hours between symptom onset and treatment dramatically reduces any chance of partial vision recovery. The National Eye Institute classifies CRAO as an ocular emergency equivalent in urgency to a brain stroke. Call 911 or go directly to an emergency department. Do not wait for an optometry appointment.
Diagnosis: What Doctors Check
Eye Examination
Fundus examination (looking into the back of the eye with a dilated pupil) reveals cherry-red spots in CRAO, retinal hemorrhages in RVO, and sometimes visible Hollenhorst plaques in the artery. This exam takes minutes and provides immediate diagnostic information.
Imaging (OCT, Angiography)
Optical coherence tomography (OCT) shows retinal swelling layer by layer without radiation. Fluorescein angiography involves injecting dye into a vein and photographing how it moves through retinal vessels, identifying the exact blockage location and extent of non-perfused retina.
Blood Tests and Vascular Evaluation
Blood tests check for clotting disorders, cholesterol levels, inflammatory markers (specifically ESR and CRP for giant cell arteritis, a serious eye stroke cause in adults over 70), and HbA1c for diabetes. Carotid artery ultrasound checks for plaque that could be sending emboli to the eye.
FAQs
What is an eye stroke and how does it happen?
An eye stroke is a blockage of the central retinal artery or vein that cuts blood supply to the retina. It happens when a blood clot, cholesterol embolus, or vessel wall damage blocks blood flow. The retina begins dying within 4-6 minutes. It causes sudden, painless vision loss in one eye.
What causes sudden vision loss in one eye stroke?
Sudden vision loss in one eye results from a stroke, which is caused by central retinal artery occlusion (CRAO), where a clot or embolus blocks the main artery feeding the retina. 74% of CRAO patients present with vision of 20/400 or worse. Loss occurs within seconds to minutes and is painless, which causes many patients to delay seeking care.
How to restore vision after an eye stroke?
The restoration of vision after eye stroke depends on treatment speed. Ocular massage and anterior chamber paracentesis are used within 4 hours for CRAO. Anti-VEGF injections (bevacizumab, ranibizumab) treat retinal vein occlusion over 3-6 monthly doses. Full recovery is rare; partial improvement is the realistic outcome with fast treatment.
Is vision loss from eye stroke permanent?
Yes, in most CRAO cases. Retinal cells that die from oxygen deprivation do not regenerate. The National Eye Institute reports that fewer than 20% of CRAO patients recover useful vision even with immediate treatment. Retinal vein occlusion carries better recovery odds with anti-VEGF injections, especially when started within 3 months of symptom onset.
What are early signs of an eye stroke?
Early signs of an eye stroke include sudden blurring in one eye, a dark shadow or grey patch in part of your visual field, and complete blackout of one eye with no pain. Some patients notice brief episodes of vision loss lasting seconds (called amaurosis fugax) days before a full eye stroke occurs.
Who is at risk for an eye stroke?
Adults over 60 with high blood pressure, diabetes, high cholesterol, or glaucoma face the highest risk. Diabetics have a 3.4 times higher retinal vein occlusion risk than non-diabetics. Women taking oral contraceptives with a migraine history also carry elevated risk due to combined effects on clotting and vascular inflammation.
How is an eye stroke diagnosed?
An eye stroke is diagnosed through fundus examination, which reveals cherry-red spots (CRAO) or retinal hemorrhages (RVO). OCT imaging measures retinal swelling. Fluorescein angiography maps blood flow blockage. Blood tests check clotting disorders, HbA1c, and inflammatory markers. Carotid ultrasound identifies arterial plaque sending emboli to the eye.
When should you seek emergency care for vision loss?
Seek emergency care immediately, within the first hour, when vision loss in one eye is sudden, painless, and affects part or all of your visual field. Do not wait for an eye appointment. CRAO has a 4-hour treatment window. Every hour of delay reduces the chance of partial vision recovery in an eye stroke event.