Blood pressure level of stroke risk is 180/120 mmHg or higher. At this threshold, the American Heart Association classifies the situation as a hypertensive emergency, where brain arteries face enough pressure to rupture or trigger a clot within hours. High blood pressure causes nearly 50% of all strokes in the US and kills around 685,000 Americans each year.
High blood pressure is the most preventable cause of stroke in the US. The numbers are measurable. The risks are specific. The interventions work when applied consistently. Check the readings, know the thresholds, and act before the body forces the decision.
Dangerous Blood Pressure Numbers for Stroke
Dangerous blood pressure numbers for stroke begin earlier than most people expect. A sustained reading of 130/80 mmHg already doubles long-term stroke risk compared to a healthy 120/80 mmHg. The immediate crisis zone starts at 180/120 mmHg, where stroke risk in the next 24 hours rises sharply.
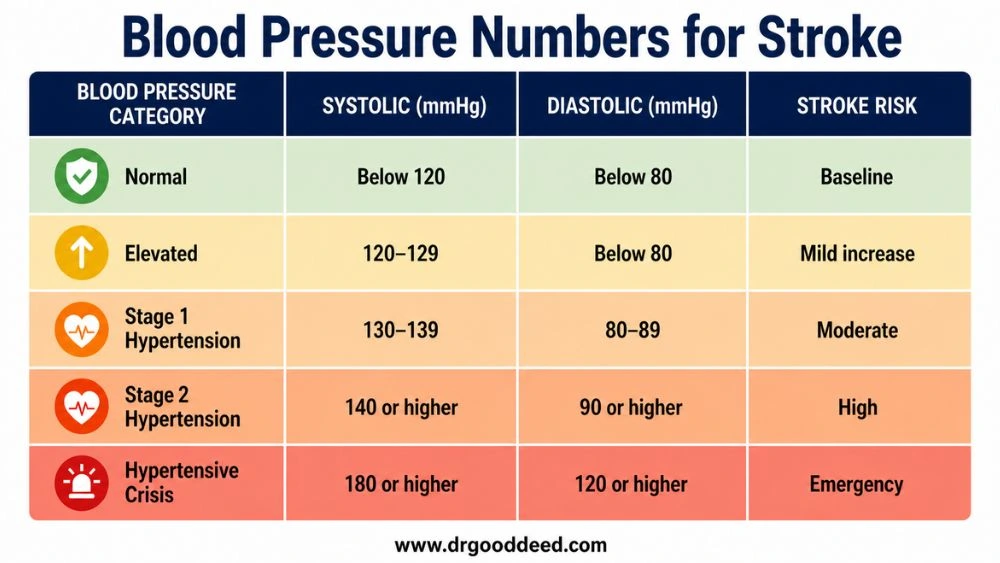
The Framingham Heart Study found stroke risk doubles for every 20 mmHg increase in systolic pressure above 115 mmHg. The table below shows where each category sits on that risk scale.
| Blood Pressure Category | Systolic (mmHg) | Diastolic (mmHg) | Stroke Risk |
| Normal | Below 120 | Below 80 | Baseline |
| Elevated | 120-129 | Below 80 | Mild increase |
| Stage 1 Hypertension | 130-139 | 80-89 | Moderate |
| Stage 2 Hypertension | 140 or higher | 90 or higher | High |
| Hypertensive Crisis | 180 or higher | 120 or higher | Emergency |
Blood Pressure Levels That Can Cause Stroke
Blood pressure levels that can cause stroke aren’t limited to the crisis range. Sustained readings above 140/90 mmHg damage arteries silently over months and years, setting the stage for stroke even when the person feels fine. Knowing Blood pressure level of stroke requires understanding both acute spikes and long-term damage.
Long-Term High Blood Pressure Damage
Chronic hypertension above 140/90 mmHg stiffens artery walls through a process called arterial remodeling. Smooth muscle cells in artery walls thicken in response to constant pressure. Over years, those walls lose their elasticity and become brittle. Brittle brain arteries rupture easily under stress causing hemorrhagic stroke.
A 2021 analysis published in The Lancet confirmed that every 10 mmHg reduction in systolic blood pressure reduces stroke risk by about 27%.
Sudden Spikes Leading to Stroke
Many strokes happen not from permanently elevated readings, but from a sudden spike. Blood pressure surges naturally in the morning, typically 20 to 25 mmHg above the overnight low. This “morning surge” explains why most strokes occur between 6 AM and 10 AM.
Emotional stress, intense physical exertion, or stimulant use can push BP to 180/120 or higher within minutes, even in people with otherwise stable readings.
Chronic Hypertension Increasing Risk Over Time
Sustained stage 2 hypertension causes “silent strokes,” also called lacunar infarcts. These are tiny blockages in small brain arteries with no dramatic symptoms. The person feels fine. But these accumulate quietly over time, leading to cognitive decline, chronic weakness, and eventually a major stroke.
How Hypertension Damages Blood Vessels
Hypertension damaging blood vessels is a step-by-step process. It explains why high BP is dangerous even when someone feels completely healthy.
Weakening of Artery Walls
Persistent high pressure stresses the inner lining of arteries, called the endothelium. Micro-tears form. The body patches them with scar tissue. Over time, that scar tissue stiffens the artery wall. Stiff brain arteries rupture under pressure far more easily than healthy flexible ones.
Narrowing and Blockage (Atherosclerosis)
High blood pressure accelerates atherosclerosis, the buildup of fatty plaques inside arteries. Plaques narrow the blood channel. When a plaque ruptures, it releases material that immediately triggers a clot, blocking blood flow to the brain entirely. That is an ischemic stroke. Ischemic strokes account for approximately 87% of all strokes in the US, and atherosclerosis driven by hypertension is the primary driver.
Increased Risk of Clot Formation or Rupture
Hypertension damaging blood vessels goes beyond plaques. Sustained high pressure activates platelets, making blood clot more readily even without a rupture. At the same time, tiny vessels in the brain called arterioles weaken under repeated pressure until they burst without warning. This is how hypertensive hemorrhagic stroke happens.
Dizziness and High BP Stroke Symptoms
Dizziness and high BP stroke symptoms overlap enough to cause confusion. Not all dizziness signals a stroke, but sudden dizziness combined with any other symptom on this list means call 911 without delay.
Most people know the FAST acronym (Face drooping, Arm weakness, Speech difficulty, Time to call 911). What most articles don’t mention is the expanded version: BE-FAST, which adds Balance and Eyes. Sudden balance loss and sudden vision changes are early stroke signs that often appear before the classic FAST symptoms develop.
Sudden Dizziness or Imbalance
Stroke-related dizziness hits in seconds with no positional trigger. It comes from reduced blood flow to the cerebellum or brainstem. Unlike standard vertigo, it doesn’t improve when the person lies down.
Severe Headache
A stroke-level headache reaches maximum intensity within 60 seconds. Neurologists call it a “thunderclap.” It signals a hemorrhagic stroke, where a vessel in or around the brain has ruptured.
Blurred Vision
Sudden vision loss or double vision in one or both eyes, lasting more than a few seconds, points to interrupted blood flow to the visual cortex or the optic nerve pathway.
Weakness or Numbness
One-sided facial drooping, arm weakness, or leg numbness that appears suddenly are classic ischemic stroke signs. If a person can’t hold both arms at shoulder height without one drifting downward, that arm drift is a clinically recognized stroke indicator.
When High Blood Pressure Becomes an Emergency
Hypertensive Crisis Symptoms
A hypertensive crisis is a reading at or above 180/120 mmHg. Two subtypes exist: urgent (high BP alone, no organ damage yet) and emergency (high BP with active organ damage happening now). Stroke is a hypertensive emergency. So is aortic dissection and acute heart attack.
Chest Pain, Confusion, or Vision Loss
When high BP arrives alongside chest pain, sudden confusion, severe headache, or vision loss, that combination signals end-organ damage already in progress. Do not wait to see if it passes.
Immediate Risk of Stroke
Blood pressure level of stroke risk is truly immediate at 180/120 mmHg combined with any neurological symptom, the stroke window narrows to hours. The American Stroke Association reports that every minute of delayed treatment during stroke costs approximately 1.9 million neurons.
How to Lower Blood Pressure to Prevent Stroke
Lowering blood pressure to prevent stroke requires consistent daily action, not one-time changes.
- Reduce sodium to under 2,300 mg daily; below 1,500 mg provides even stronger protection for stage 2 hypertension
- Follow the DASH diet; clinical trials show it reduces systolic BP by 8 to 14 mmHg
- Get 150 minutes of moderate aerobic exercise weekly, which lowers systolic BP by 5 to 8 mmHg
- Lose 1 kg of body weight to reduce systolic BP by approximately 1 mmHg
- Limit alcohol to one drink daily for women, two for men
- Take prescribed antihypertensives daily without skipping; missed doses cause rebound spikes
- Monitor BP every morning before eating or taking medications, and log the readings
- Manage stress actively, because cortisol raises blood pressure within minutes of a stress response
Who Is at Highest Risk of Stroke from High BP
Blood pressure levels that can cause stroke affect some groups far more severely. These populations face the steepest risk:
- African Americans in the US develop hypertension earlier and at higher rates, with stroke mortality nearly twice that of white Americans
- Adults over 65 with isolated systolic hypertension (systolic above 140, diastolic below 90) face a 2x to 3x elevated stroke risk
- People with diabetes and high BP together face stroke risk approximately 4x above baseline due to compounding vascular damage
- People with atrial fibrillation and hypertension; this combination accounts for a significant share of embolic strokes
- Smokers with high BP; smoking adds direct endothelial damage on top of arterial stiffening
FAQs
What are dangerous blood pressure numbers for stroke?
Dangerous blood pressure numbers for stroke begin at 140/90 mmHg for long-term risk. The immediate emergency threshold is 180/120 mmHg. The Framingham Heart Study confirmed stroke risk doubles for every 20 mmHg rise in systolic pressure above 115 mmHg, so even moderate elevations matter over time.
Can slightly high blood pressure cause strokes?
Yes. Sustained BP above 130/80 mmHg causes silent lacunar infarcts, tiny brain strokes with no obvious symptoms. Over years, they accumulate into measurable cognitive decline and permanent neurological damage, well before a dramatic full stroke occurs.
How does hypertension damage blood vessels?
Hypertension damages blood vessels, following three stages: endothelial micro-tears trigger scar buildup, chronic pressure accelerates plaque formation inside arteries, and repeated pressure spikes activate platelet clotting. All three occur simultaneously in untreated hypertension, each independently raising stroke risk.
What are dizziness and high BP stroke symptoms?
Dizziness and high BP stroke symptoms include sudden loss of balance, one-sided facial drooping, arm weakness, slurred speech, vision changes in one or both eyes, and a thunderclap headache reaching peak intensity within 60 seconds. Dizziness alone is not diagnostic. With any other symptom, call 911 immediately.
How to lower blood pressure to prevent stroke?
Lower blood pressure to prevent stroke: follow the DASH diet, limit sodium to 1,500 to 2,300 mg daily, exercise 150 minutes weekly, lose weight progressively, and take antihypertensives without skipping. Combined lifestyle changes can reduce systolic BP by 15 to 20 mmHg, the equivalent of one medication.
When does high blood pressure become an emergency?
At 180/120 mmHg. If that reading comes with chest pain, confusion, vision loss, severe headache, or any neurological symptom, go to an emergency room immediately. Do not take an extra BP medication and wait. That is a hypertensive emergency with active organ damage in progress.
Can strokes happen without very high blood pressure?
Yes. Strokes happen with normal BP when atrial fibrillation sends clots to the brain, when carotid plaques rupture spontaneously, or during arterial dissection. Blood pressure level of stroke risk depends on context; BP is a major factor but not the only one.
How often should I check my blood pressure?
Check it every morning before eating or taking medications. People with stage 1 or 2 hypertension should check daily and log the readings. A single clinic reading misses the morning surge, the nocturnal dip pattern, and white-coat effects that home monitoring consistently captures.
When should I see a doctor for high BP?
See a doctor immediately if home readings consistently exceed 140/90 mmHg over two weeks. Go to an ER if any single reading exceeds 180/120 mmHg, with or without symptoms. Blood pressure level of stroke damage begins before pain or warning signs appear.